Stellate Ganglion Block
Author
Michael Gofeld, MD
Assistant Professor
University of Washington School of Medicine
Commentary
Bernhard Moriggl, MD
Professor
Innsbruck Medical University
Innsbruck, Austria
Introduction
First described by Leriche in the 1930s,[1] the stellate ganglion block (SGB) has been in use since that time without significant modification as a diagnostic and therapeutic intervention in chronic regional pain syndromes of the upper extremities[2-3] as well as for a variety of medical conditions such as vascular insufficiency, post-herpetic neuralgia, phantom pain, vascular headache, cardiac arrhythmia, to name a few.[4]
Anatomy
Virtually all the sympathetic innervation of the head, neck and upper extremities passes through the stellate ganglion.[5] Preganglionic sympathetic fibers originate from cell bodies in the anterolateral column of the spinal cord.[6] Axons from these cell bodies travel via the anterior roots of the spinal cord and join the superior, middle, intermediate and inferior cervical sympathetic ganglia. In 80% of individuals the inferior cervical ganglion is fused with the first thoracic ganglion, forming the stellate ganglion, whose oval shape measures 2.5 cm long, 1 cm wide and 0.5 cm thick.[5] It is usually located behind the subclavian artery in front of the first rib[4] and lateral to the longus colli muscle. There is a great anatomic variability in the ganglion shape and appearance.[7] Other key structures adjacent to the stellate ganglion include the esophagus and trachea, which lie medial, and the vertebral artery which lies anterior. From the stellate ganglion, post-ganglionic fibers are sent to the cervical nerves (C7-C8) and first thoracic nerve (T1) to provide sympathetic innervation to the upper limbs.[5-6] The preganglionic fibers of the head and neck continue to travel cephalad to the superior and middle cervical ganglion through the sympathetic chain. Stellate ganglion block interrupts the sympathetic outflow to the head and neck by inactivation of the preganglionic fibers and/or postganglionic fibers from the ganglion itself.[8]
Traditional Techniques
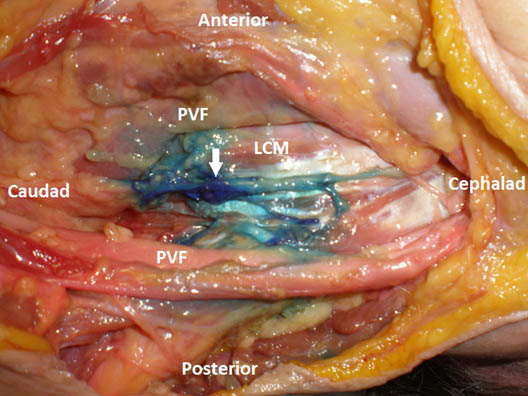 Figure 1. Cadaver dissection. Methylene blue (0.2 mL) injected subfascially staining the sympathetic trunk (white arrow). LCM = longus colli muscle; PVF = prevertebral fascia
Figure 1. Cadaver dissection. Methylene blue (0.2 mL) injected subfascially staining the sympathetic trunk (white arrow). LCM = longus colli muscle; PVF = prevertebral fascia
While several methods of stellate ganglion blockade have been described, the most popular approach is the classical technique using the anatomical landmark of the prominent anterior tubercle of C6 transverse process (Chassaignac’s tubercle). A needle is advanced perpendicular to the skin while retracting the sternocleidomastoid muscle along with the internal carotid artery until bony contact is made with the tubercle of C6 transverse process. Different volumes of local anesthetics are recommended in the literature[9] ranging from 5–20 mL. There is no single accepted test to confirm successful block, although the presence of Horner’s syndrome and elevation in skin temperature of the upper extremities by 1–3°C are commonly used.[10]
The above technique relies on accurate localization of the C6 tubercle, despite the fact that the ganglion itself lies at the level of the first rib. As a recent anatomical study demonstrates, there is large variability in the size and location of the landmarks used to localize C6.[11] Furthermore, there is a significant risk of vertebral artery damage due to the narrow dimensions of the transverse process (6 mm) in the cephalad to caudad direction. While the use of X-rays minimizes the risk,[12] precise location of the cervical sympathetic trunk is defined by the fascial plane of the prevertebral fascia, and this cannot be resolved by means of fluoroscopy. Vascular structures (the inferior thyroid, the vertebral and carotid arteries) and soft tissues (the thyroid gland and esophagus) are also not seen with fluoroscopy and are therefore at risk of puncture with a fluoroscopy-guided technique.[13] Lateral deviations of the needle may result in contact with the posterior tubercle where an injection of local anesthesia can result in a transforaminal injection.[11]
Studies to define anatomic distribution of injections performed at C6 have produced conflicting results due to the limitations of the techniques employed.[14-17] Spread of local anesthetics depends on the needle tip position either anterior or posterior to the prevertebral fascia. Injections posterior to the prevertebral fascia are associated with direct deposition of an injectate onto the sympathetic trunk (Figure 1) and greater caudal spread of local anesthetic.[15][18] High failure rate of the classical technique of SGB is possibly related to inconsistent position of the needle tip in relation to the fascial planes.[14][19] Higher volumes of injectate, which may block the stellate ganglion by overflow or diffusion, are associated with a higher risk of hoarseness secondary to contact with the recurrent laryngeal nerve[13-15] and somatic blocks of the brachial plexus.[15]
Ultrasound Techniques
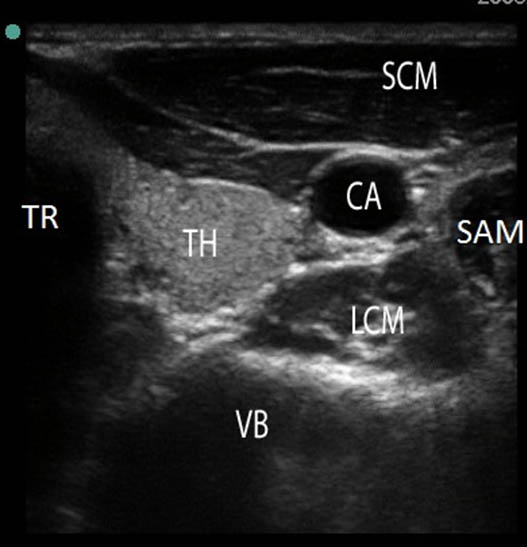
Figure 2. Sonography performed with a high-frequency linear transducer positioned at the level of the cricoid cartilage. TR = trachea; TH = thyroid gland; CA = carotid artery; SCM = sternocleidomastoid muscle; SAM = scalenus anterior muscle; LCM = longus colli muscle; VB = vertebral body.
Anterior Approach
The patient is placed in the supine position with the neck in slight extension. A high frequency linear transducer is placed at the level of the cricoid cartilage to allow cross-sectional visualization of anatomic structures, including the C6 vertebral body, longus colli muscle, prevertebral fascia, carotid artery and thyroid gland (Figure 2).
Alternatively a low frequency curved transducer may be used to obtain a “panoramic view” (Figure 3). A pre-scan is important in planning the path of needle insertion as the presence of the esophagus[13] and the inferior thyroidal artery[13] may obviate the needle insertion path between the carotid artery and trachea. In that situation, the needle may be inserted lateral to the carotid artery.
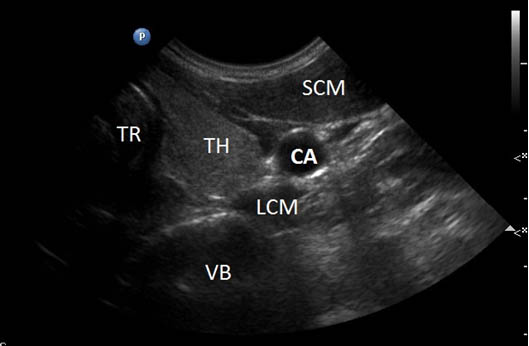 Figure 3. Sonography performed with a low-frequency curvilinear transducer at the level of the cricoid cartilage providing a wide-angle view. TR = trachea; TH = thyroid; CA = carotid artery; SCM = sternocleidomastoid muscle; LCM = longus colli muscle; VB = vertebral body.
Figure 3. Sonography performed with a low-frequency curvilinear transducer at the level of the cricoid cartilage providing a wide-angle view. TR = trachea; TH = thyroid; CA = carotid artery; SCM = sternocleidomastoid muscle; LCM = longus colli muscle; VB = vertebral body.
The tip of the needle is directed under the prevertebral fascia superficial to the longus colli muscle (video clip 1). This target point is desirable because 1) a suprafascial injection results in the spread of injectate around the carotid sheath with medial, posterior, or anterior extension, increasing the risk of hoarseness, probably secondary to local anesthetic spread to the recurrent laryngeal nerve medial to the carotid and lateral to the trachea;[15] and 2) the subfascial injection results in more caudal spread of the injectate towards the stellate ganglion.[15][18] Care must be taken to visualize the spread of injectate under real-time scanning. Absence of injectate spread may suggest inadvertent intravascular injection.
Lateral Technique
Patient is placed at a lateral decubitus position with the block side up. Short-axis ultrasonography is performed from the cricoid cartilage posteriorly (Figure 4). After localizing the carotid artery and the internal jugular vein, the C6 transverse process can be seen in its typical appearance. It has a prominent anterior tubercle and a shorter posterior tubercle. The exiting C6 nerve root is visualized as a round hypoechoic structure between the tubercles. The longus colli muscle is seen as an oval structure adjacent to the base of the transverse process and vertebral body. Sometimes the caudal portion of the longus capitis muscle could be seen as well. The C7 transverse process can be found immediately caudad to the C6. Unlike the C6 transverse process, the C7 transverse process has no anterior tubercle. The C7 nerve root was situated just anterior to the transverse process (Figure 5).
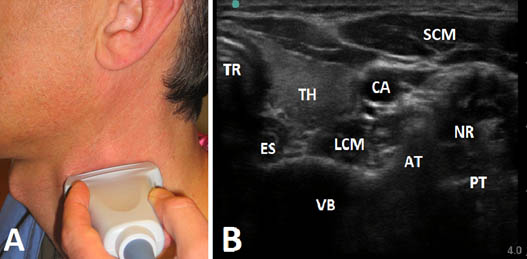 Figure 4. Sonography of the anterolateral aspect of the neck at the C6 transverse process. A) Position of the transducer B) Sonogram. TR = trachea; ES = esophagus; TH = thyroid; CA = carotid artery; SCM = sternocleidomastoid muscle; LCM = longus colli muscle; VB = vertebral body; N = nerve root; AT = anterior tubercle; PT = posterior tubercle.
Figure 4. Sonography of the anterolateral aspect of the neck at the C6 transverse process. A) Position of the transducer B) Sonogram. TR = trachea; ES = esophagus; TH = thyroid; CA = carotid artery; SCM = sternocleidomastoid muscle; LCM = longus colli muscle; VB = vertebral body; N = nerve root; AT = anterior tubercle; PT = posterior tubercle.
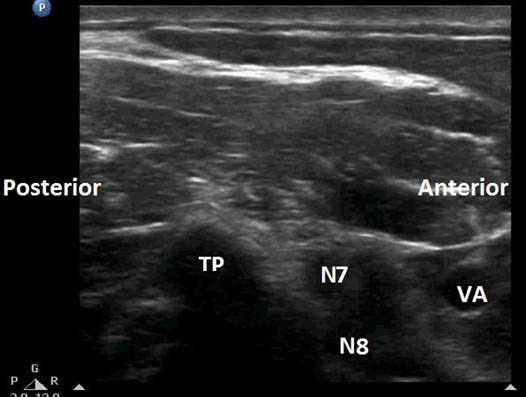
Figure 5. Transverse sonogram of the anterolateral aspect of the neck at the level of C7 transverse process. TP = transverse process; VA = vertebral artery; N7 = seventh cervical nerve root; N8 = eighth cervical nerve root.
At the C6 level a spindle-shaped structure can be localized on the short-axis view in 30% of cases (the middle cervical ganglion). It is typically situated on the anterolateral surface of the longus colli muscle; if the ganglion could not be identified, some widening of the tissue plane below the prevertebral fascia could usually be appreciated.
When clear picture of pertinent anatomy is obtained the transducer should be moved slightly anteriorly until only the anterior tubercle of the C6 transverse process is visible adjacent to the projected entry point of the needle, and no visceral or neural elements are situated on the line connecting the entry site and the lateral surface of the longus colli muscle (Figure 6).
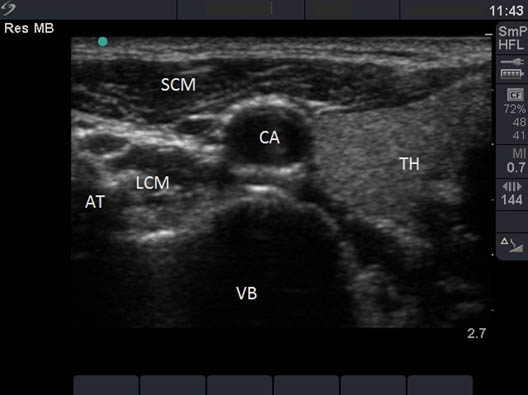 Figure 6. Sonogram of the anterolateral neck at the level of C6. AT = anterior tubercle; LCM = longus colli muscle; VB = vertebral body; CA = carotid artery; SCM = sternocleidomastoid muscle; TH = thyroid.
Figure 6. Sonogram of the anterolateral neck at the level of C6. AT = anterior tubercle; LCM = longus colli muscle; VB = vertebral body; CA = carotid artery; SCM = sternocleidomastoid muscle; TH = thyroid.
Occasionally the internal jugular vein is seen within the projected needle track, but it could be collapsed readily under light transducer pressure. Typically the needle passage is entirely intramuscular, i.e., through the sternocleidomastoid muscle or the anterior scalene muscle or both. Under real-time ultrasound guidance, a block needle is inserted via the “lateral pathway” using the in-plane technique (Figure 7).
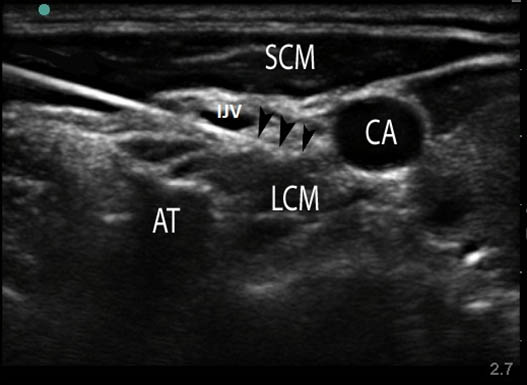
Figure 7. Sonogram of the anterolateral neck at the level of C6: needle inserted using an in-plane lateral approach. AT = anterior tubercle; IJV = collapsed internal jugular muscle; SCM = sternocleidomastoid muscle; LCM = longus colli muscle; CA = carotid artery.
The author recommends double syringe injection technique. Two syringes are connected to the needle by means of a three-way stopcock and extension tubing; the first syringe contains NaCl 0.9% and the second contains a local anesthetic. Once placement of the needle had been confirmed, 1–2 mL of NaCl should be injected to confirm subfascial placement of the needle. The NaCl allowed clear separation of the tissue planes (video clip 2). If the spread is appropriate, 5 mL of local anesthetic is injected.
Literature Review
Kapral et al.[20] compared ultrasound-guided stellate ganglion block with the blind injection. These authors used a lower volume of local anesthetic (5 mL rather than 8 mL) for the ultrasound technique. The ultrasound technique did not result in hematoma (as opposed to 3 in the blind injection group), and was associated with a more rapid onset of Horner’s syndrome. However, since tissue visualization was probably not feasible below the C7 level, these authors concluded that a local anesthetic depot was limited to the C4–C7 levels and speculated that upper extremity sympathetic blockade was not related to blockade of the stellate ganglion per se.
Shibata et al.[21] suggested that subfascial injection would result in better spread of the injectate and a more reliable sympathetic blockade. The published image is ambiguous and it is not clear whether subfascial or intramuscular injection was actually performed. Narouze at al.[13] further emphasized the risks of a blind approach at the C6 level e.g., accidental esophageal puncture particularly on the left side. In addition, the needle traverses the thyroid gland and the inferior thyroid artery may cause a hematoma formation.
Gofeld at al.[18] performed a combined preclinical-clinical study with imaging validation and confirmed subfascial location of the sympathetic trunk. The lateral technique with injection of 5 ml of a local anesthetic performed at C6 level will result in reliable spread of the injectate onto the stellate ganglion. This study also claimed improved safety when the injection performed laterally to the carotid sheath and the thyroid gland.
Commentary
Classification of Procedure
This is considered an intermediate (level 2) block (intermediate). Although traditionally named a stellate ganglion block it is in reality a cervical sympathetic trunk block.
Transducer Frequency
A curved array transducer with a small footprint (”microconvex transducer”) and medium frequency may be very useful. However, the cervical sympathetic trunk itself may not be visible when a medium frequency transducer is used.
Additional Anatomical Remarks
The stellate ganglion (SG), if present, extends from the level of the head of the first rib to the inferior border of the transverse process of C7. It lies medial (more often) or posterior to the origin of the vertebral artery and immediately adjacent to the dome of pleura! It is thus understandable why the block is usually performed more cranially at the level of the transverse process of C6 (which often includes part of the middle cervical ganglion) to avoid complications. The primary target in this case is the cervical sympathetic trunk at that level. Blockade of the SG is only indirectly achieved by virtue of inferior spread of local anesthetic depending on the volume injected.
The cervical sympathetic trunk (CST) is situated prevertebral. That is, the upper part of the CST (including the superior ganglion) rests on the longus capitis muscle, the middle part of the CST (where block is usually done) on the longus colli muscle with close relationship to the inferior thyroid artery, and the inferior part of the CST (including inferior cervical ganglion and SG, respectively) is found at the lateral border of longus colli muscle and within the vertebro-scalene triangle, respectively.
The CST itself is deep to the “prevertebral fascia” that separates the CST from the neurovascular bundle in front i.e., the internal carotid artery, common carotid artery, internal jugular vein, and vagus nerve.
There are many anatomical variabilities. For example, the middle cervical ganglion may be absent. The CST may be split into 2-3 very thin subdivisions. In both cases, ultrasound detection will be very challenging. Also, the middle cervical ganglion may be ventral to the inferior thyroid artery. The dimensions of both the ganglia and the interganglionic branches can be highly variable. There may be a separate inferior cervical ganglion and a 1st thoracic ganglion without a true SG!
Sono-anatomical Considerations
The CST appears in ultrasound images as either a flat or spindle shaped neural structure (always smaller than the vagus nerve which is round). If present, the middle cervical ganglion may appear oval and in most cases it is found at the C5 level. The echogenicity of both the CST and middle cervical ganglion may vary (not the least due to artifacts).
Common Ultrasound Guided Technical Errors
Possible errors are:
- Scanning may be too caudal searching for the true stellate ganglion.
- Needle tip is placed anterior to the deep cervical fascia.
- Injection is too deep into the longus colli muscle.
- The CST may be confused with the vagus nerve or small lymph nodes.
- Sonographic topography can be altered with different head positions. The position of the neurovascular bundle (carotid artery, internal jugular vein and vagus nerve) changes when the head is turned while the CST position does not change. In addition, the neurovascular bundle can easily be pushed to one side or the other by simply increasing the transducer pressure on the skin. This is particularly true with the use of a microconvex transducer.
References
- Leriche R, Fontaine R. isolee du ganglion etoile. Sa technique, ses indications, ses resultats. Presse Med 1934;41:849-850
- Raj PP. Stellate ganglion block. In: Waldman SD, Winne AP (eds). Interventional Pain management. Philaelphia, Dannemiller Education, WB Saunders Co., 1996.
- Stanton-Hicks MD, Burton AW, Bruehl SP, et al. An updated interdisciplinary clinical pathway for CRPS: report of an expert panel. Pain Pract 2002;2:1-16.
- Elias M. Cervical sympathetic and stellate ganglion blocks. Pain Physician 2000;3:294-304.
- Hogan QH, Erickson S. MR imaging of the stellate ganglion: normal appearance. AJR 1992;158:655-659.
- Tubbs RS, Loukas M, Remy AC, et al. The vertebral nerve revisited. Clin Anat 2007;20:644-647.
- Slappendel F, Thijssen H, Crul BJ, et al. The stellate ganglion in magnetic resonance imaging, a quantification of anatomic variability. Anesthesiology 1995;83:424-426.
- Cepeda MS, Lau J, Carr DB. Defining the therapeutic role of local anesthetic sympathetic blockade in complex regional pain syndrome: a narrative and systematic review. Clin J Pain 2002;18:216-233.
- Feigl GC, Rosmarin W, Stelzl A, et al. Comparison of different injectate volumes for stellate ganglion block: an anatomic and radiologic study. Reg Anesth Pain Med 2007;32:203-208.
- Malmqvist EL, Bengtsson M, Sorenson J. Efficacy of stellate ganglion block: A clinical study with bupivacaine. Reg Anesth 1992;17:340-347.
- Janik JE, Hoeft MA, Ajar AH, et al. Variable osteology of the sixth cervical vertebra in relation to stellate ganglion block. Reg Anesth Pain Med 2008;33:102-108.
- Abdi S, Zhou Y, Patel N, et al. A new and easy technique to block the stellate ganglion. Pain Physician 2004;7:327-331.
- Narouze S, Vydyanathan A, Patel N. Ultrasound-guided stellate ganglion block successfully prevented esophageal puncture. Pain Physician 2007;10:747-752.
- Hardy PAJ, Wells JCD. Extent of sympathetic blockade after stellate ganglion block with bupivacaine. Pain 1989;36:193-196.
- Christie JM, Martinez CR. Computerized axial tomography to define the distribution of solution after stellate ganglion nerve block. J Clin Anesth 1995;7:306-311.
- Erickson SJ, Hogan QH. CT-guided injection of the stellate ganglion: description of technique an defficacy of sympathetic blockade. Radiology 1993;188:707-709.
- Honma M, Murakami G, Sato TJ, et al. Spread of injectate during C6 stellate ganglion block and fascial arrangement in the prevertebral region: an experimental study using donated cadavers. Reg Anesth Pain Med 2000;25:573-583.
- Gofeld M, Bhatia A, Abbas S, Ganapathy S, Johnson M. Development and validation of a new technique for ultrasound-guided stellate ganglion block. Reg Anesth Pain Med 2009;34:475-479.
- Hogan QH, Taylor, ML, Goldstein M, et al. Success rates in producing sympathetic blockade by paratracheal injection. Clin J Pain 1994;10:139-145.
- Kapral S, Krafft P, Gosch M, et al. Ultrasound imaging for stellate ganglion block: direct visualization of puncture site and local anesthetic spread. Reg Anesth 1995;20:323-328.
- Shibata Y, Fujiwara Y, Komatsu T. A new approach of ultrasound-guided stellate ganglion block. Anesth Analg 2007;105:550-551.