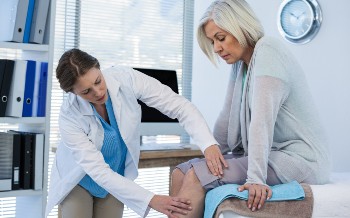
 Total knee replacement is one of the most common surgeries in the United States.[1] Almost 700,000 procedures were performed in 2010,[1] and this number is expected to increase in the future.[2] If you are one of the many patients who need a knee replacement, a physician anesthesiologist will help you through the surgery. You will start with an assessment before your operation (preoperative assessment), and your anesthesiologist will work with you and your surgeon to choose the best type of anesthesia for the surgery. After the surgery, the anesthesiologist and surgeon will do their best to make sure you have as little pain as possible while also making sure your leg motion and walking ability are the best they can be.
Total knee replacement is one of the most common surgeries in the United States.[1] Almost 700,000 procedures were performed in 2010,[1] and this number is expected to increase in the future.[2] If you are one of the many patients who need a knee replacement, a physician anesthesiologist will help you through the surgery. You will start with an assessment before your operation (preoperative assessment), and your anesthesiologist will work with you and your surgeon to choose the best type of anesthesia for the surgery. After the surgery, the anesthesiologist and surgeon will do their best to make sure you have as little pain as possible while also making sure your leg motion and walking ability are the best they can be.
What Will Happen During the Preoperative Assessment?
Before surgery, your anesthesiologist will go over your medical history. You will be asked about any medical problems you may have, your previous surgeries, what medicines you are taking, what you are allergic to, your social habits (smoking, alcohol, recreational drugs), the last time you ate or drank anything, and any problems you may have had with anesthesia in the past. Your anesthesiologist will also examine your mouth and neck and listen to your heart and lungs. Depending on your medical history, you may need your blood drawn or have other tests done to get you ready for surgery.[3]
It is very important to answer all questions honestly and as completely as you can. The anesthesiologist uses this information to plan your care, so it is important to be as accurate as possible. If you have a lot of allergies or take a lot of medicines, it can be helpful to write out a list ahead of time.
You may be given medicine in the preoperative area before you go to surgery. Antibiotics, medicine to help you relax, and medicine for pain are often given at this time.[3] At many centers, you may also receive a nerve block before surgery to help you with your pain after surgery.
Pain After Surgery
During a total knee replacement, your knee joint is taken out and replaced with metal and plastic parts. This will be painful, and the pain can last for days to weeks. At the same time, it is important to get up and about soon after surgery to help with recovery. It is also very important to start physical therapy. Pain can interfere with your mobility and delay your recovery, so your surgeon and anesthesiologist take pain relief very seriously.[4]
Opioids (narcotics) have traditionally been used for pain relief after surgery. They can be given by injection or by mouth. They can be given by nurses, or patients can give themselves doses as needed using something called patient-controlled analgesia. Unfortunately, opioids have many unwanted side effects including drowsiness, slowed breathing, constipation, nausea, vomiting, itching, and difficult urination in addition to the potential for addiction. Other pain medicines may be mixed in with opioids (multimodal analgesia) in order to reduce unwanted side effects while still relieving pain after surgery.[5]
What Is Multimodal Analgesia?
Multimodal analgesia, which may be administered before and/or after surgery, means using several different types of medicine that work in different ways at the same time to relieve pain. The combination gives better pain relief than any one thing by itself and reduces side effects.[4]
Nerve blocks can be an important part of multimodal analgesia after knee replacement surgery.[6] To understand how they work, it is helpful to understand what nerves are and what they do.
What Are Nerves?
.jpg?sfvrsn=c2aeaf3a_2) Nerves are the body’s communication system. They carry messages back and forth between the brain and spinal cord and the rest of the body. The brain controls the body by sending signals along nerves to tell the body what to do. Signals carrying information about touch, taste, smell, and other sensations travel from the body to the brain. When part of your body is hurt, signals travel along the nerves to the brain, and you feel pain. Nerves travel throughout the body in small bundles.[7] You can think of nerves as the body’s telephone lines or television cables.
Nerves are the body’s communication system. They carry messages back and forth between the brain and spinal cord and the rest of the body. The brain controls the body by sending signals along nerves to tell the body what to do. Signals carrying information about touch, taste, smell, and other sensations travel from the body to the brain. When part of your body is hurt, signals travel along the nerves to the brain, and you feel pain. Nerves travel throughout the body in small bundles.[7] You can think of nerves as the body’s telephone lines or television cables.
What Is a Nerve Block?
A nerve block is a way to block the signals that travel along nerves. Your anesthesiologist can inject local anesthetic (“numbing medication”) near the nerves. The anesthetic blocks the signals and keeps the pain sensation from reaching the brain.[6] Your anesthesiologist may offer you one or more nerve blocks to help you feel less pain after your surgery. Examples include the femoral nerve block and adductor canal (saphenous nerve) block.What Is a Nerve Block?
Femoral Nerve Block
.jpg?sfvrsn=b0f459f_2) A femoral nerve block is often used to help with pain relief after total knee replacement.[4] You will lie on your back for this block. The anesthesiologist will clean the skin around your groin and inject some local anesthetic to numb the skin. He or she will then slowly put in the block needle until it is near the femoral nerve. The anesthesiologist may use ultrasound to see the nerve and/or use a nerve stimulator to help find the right position. The stimulator uses a very small amount of electricity to make your leg muscles twitch when the needle is close to the nerve. Once the needle is in the right spot, local anesthetic is injected. A catheter can also be put in at that time to allow additional local anesthetic to be injected after surgery to extend the duration of your pain relief.[6]
A femoral nerve block is often used to help with pain relief after total knee replacement.[4] You will lie on your back for this block. The anesthesiologist will clean the skin around your groin and inject some local anesthetic to numb the skin. He or she will then slowly put in the block needle until it is near the femoral nerve. The anesthesiologist may use ultrasound to see the nerve and/or use a nerve stimulator to help find the right position. The stimulator uses a very small amount of electricity to make your leg muscles twitch when the needle is close to the nerve. Once the needle is in the right spot, local anesthetic is injected. A catheter can also be put in at that time to allow additional local anesthetic to be injected after surgery to extend the duration of your pain relief.[6]
Adductor Canal (Saphenous Nerve) Block
.jpg?sfvrsn=8d12a85a_2) This type of block is performed close to the groin where the femoral nerve block is typically performed. For this block, your leg will be turned to the side with your knee slightly bent. Your skin will be cleaned. The anesthesiologist will likely use ultrasound to find the nerve as it travels through your thigh. Some local anesthetic will be used to numb your skin. The block needle will then be positioned near the nerve. Ultrasound is commonly used to make sure the needle is in the right place. Local anesthetic will then be injected.[8] There is evidence that this block causes less muscle weakness on the first day after surgery than a femoral nerve block.[9]
This type of block is performed close to the groin where the femoral nerve block is typically performed. For this block, your leg will be turned to the side with your knee slightly bent. Your skin will be cleaned. The anesthesiologist will likely use ultrasound to find the nerve as it travels through your thigh. Some local anesthetic will be used to numb your skin. The block needle will then be positioned near the nerve. Ultrasound is commonly used to make sure the needle is in the right place. Local anesthetic will then be injected.[8] There is evidence that this block causes less muscle weakness on the first day after surgery than a femoral nerve block.[9]
Periarticular Injection
Your surgeon may also inject a combination of local anesthetic and other medicines around your knee at the end of surgery to help with pain relief.[5]
Combinations of local anesthetic blocks and pain medications that you take by mouth form the foundation of multimodal analgesia and can give excellent pain relief after total knee replacement.[5]
What Medicines are Included in “Multimodal Analgesia?”
In addition to the nerve blocks, one or more medicines might be given as part of multimodal analgesia, administered before and/or after surgery.
Acetaminophen (Tylenol®) is an important component of multimodal analgesia. It is effective and has a proven track record for safety when taken according to directions.[5]
Non-steroidal anti-inflammatory drugs (NSAIDs) are often included to help with pain management right after surgery. Ibuprofen (Advil®, Motrin®) is one example and helps fight inflammation that can cause pain.[5]
Other medicines for multimodal analgesia might include clonidine,[10] steroids,[5] or gabapentinoids like pregabalin.[5]
It is important to remember that multimodal analgesia can include many different approaches. Some blocks or medicines may not be good choices for some patients. Maybe you have a medical condition or take blood thinners that can make a spinal or epidural too dangerous. Maybe one of your medications may react with some of the pain medicines. Maybe your skin is red and inflamed over the spot where a nerve block would go. These are only a few examples. This is why your medical history is so important. Your anesthesiologist will consider your history and work with you and your surgeon to come up with a plan that is right for you.
What Kind of Anesthesia Can I Have?
The most common types of anesthesia for total knee replacement are general, spinal, and epidural.[4]
General Anesthesia
General anesthesia makes you completely unconscious for the surgery. Even though we call it “sleep,” general anesthesia is really like a coma. You will often be given some medication in the preoperative area to prepare you for general anesthesia before you go back to the operating room. In the operating room, you will move from the transport bed to the operating table and monitors will be put on. Your anesthesiologist will record your vital signs before you go to sleep. You will be given a mask with oxygen to breathe. The anesthesiologist will give you medicine through your IV to begin the anesthesia and will insert a breathing tube after you are under general anesthesia. The anesthesiologist will continue to give you anesthetic medicine, either through the IV or in the gas you breathe, the whole time you are in surgery. When the surgery is over, you will stop receiving anesthesia and you will wake up. The anesthesiologist will carefully monitor you throughout the entire surgery.[11]
Spinal Block
A spinal block is a very common type of anesthesia used to numb the lower part of the body. With a spinal block, the anesthesiologist puts numbing medicine into the spinal fluid but not the spine itself. In the operating room, your anesthesiologist will put some monitors on you before placing the block. He or she may also give you some medicine to help you relax. You will usually either sit up or lie on your side for the block. The anesthesiologist will clean your back and put a drape on you. He or she will then feel your back to find the best spot for the block. The anesthesiologist will then numb the skin with local anesthetic. You will be asked to arch your back like an angry cat to make it easier to place the small spinal needle in the right place. Try not to move during the block. When the needle is in the right spot, local anesthetic will be injected. The needle will be removed, and the lower part of your body will go numb within a few minutes.[12]
You don’t have to stay awake for the surgery when you have a spinal block. After the block is in place, the anesthesiologist can give you medicine to make you sleepy. The level of sedation can range from mild, where you are relaxed but aware of your surroundings, to deep, where you are completely asleep but breathing on your own without the need for a breathing tube.[13] You and your anesthesiologist can discuss how much or how little sedation you want. You can always ask for more if you need it. Regardless of the level of sedation, the anesthesiologist will monitor you throughout the surgery.[12]
In addition to numbing your legs during the surgery, a spinal block may help with pain relief long after surgery although the numbness usually wears off after 2 or 3 hours.[5]
Epidural
An epidural is like a spinal block in many ways. Both numb the lower part of your body. For you, the patient, the procedure to put them in is similar.[12]
There are some important differences, though. An epidural goes into a different space, and it usually takes a little longer to put in. It also takes longer for an epidural to numb your legs. Finally, with an epidural, a narrow catheter or tube is usually left in place.[12] The catheter can be left in after the surgery to help with pain.[14] Because putting in the epidural and numbing your legs takes a little longer than a spinal block, your anesthesiologist may do it in the preoperative area rather than in the operating room.
Combined Spinal-Epidural
Sometimes a spinal and an epidural are done at the same time. This takes advantage of the quick numbing action from the spinal block. Putting an epidural catheter in at the same time allows the anesthesiologist to give more medication if needed and can also help with pain after surgery.[12]
There is good evidence to show that patients who have a spinal or epidural instead of general anesthesia for knee replacement will have fewer complications after surgery.[15] This may mean a lower chance of experiencing heart or lung problems, needing a blood transfusion, or falling and hurting yourself.[16] Having a spinal or epidural may be safer especially for patients who have sleep apnea.[17]
What Can I Expect Right After Surgery?
After surgery, you will be taken to the recovery area. The anesthesiologist will tell the recovery nurse how the surgery went, and will then leave you in his or her care. The nurse will monitor you in the recovery area to make sure there are no problems.[11] He or she can call an anesthesiologist anytime if needed. If you had a nerve block, spinal, or epidural your legs may still be weak or numb right after surgery until the numbing medication wears off. Your anesthesiologist may continue to be involved in your care after surgery to help with pain management.
References
- ^ a b Centers for Disease Control and Prevention. Hospitalization for total knee replacement among inpatients aged 45 and over: United States, 2000-2010. 2015; https://www.cdc.gov/nchs/data/databriefs/db210.htm. Accessed June 5, 2017.
- ^ Kurtz S, Ong K, Lau E, Mowat F, Halpern M. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am. 2007;89(4):780-785.
- ^ a b Galway UA. Preoperative Evaluation. In: Sikka PK, Beaman ST, Street JA, eds. Basic Clinical Anesthesia. New York: Springer; 2015.
- ^ a b c d Moon TS, Aleshi P. Orthopedic Anesthesia. In: Sikka PK, Beaman ST, Street JA, eds. Basic Clinical Anesthesia. New York: Springer; 2015.
- ^ a b c d e f g h Halawi MJ, Grant SA, Bolognesi MP. Multimodal Analgesia for Total Joint Arthroplasty. Orthopedics. 2015;38(7):e616-625.
- ^ a b c Tom M, Halaszynski TM. Peripheral Nerve Blocks. In: Sikka PK, Beaman ST, Street JA, eds. Basic Clinical Anesthesia. New York: Springer; 2015.
- ^ Dictionary.com. Nerve. http://www.dictionary.com/browse/nerve. Accessed June 5, 2017.
- ^ Manickam B, Perlas A, Duggan E, Brull R, Chan VW, Ramlogan R. Feasibility and efficacy of ultrasound-guided block of the saphenous nerve in the adductor canal. Reg Anesth Pain Med. 2009;34(6):578-580.
- ^ Kim DH, Lin Y, Goytizolo EA, et al. Adductor canal block versus femoral nerve block for total knee arthroplasty: a prospective, randomized, controlled trial. Anesthesiology. 2014;120(3):540-550.
- ^ McHugh SM, Metro DG. NSAIDs and Alphs-2 Adrenergic Agonists. In: Sikka PK, Beaman ST, Street JA, eds. Basic Clinical Anesthesia. New York: Springer; 2015.
- ^ a b Sikka PK. Approach to Anesthesia. In: Sikka PK, Beaman ST, Street JA, eds. Basic Clinical Anesthesia. New York: Springer; 2015.
- ^ a b c d e Turnbull JH, Aleshi P. Spinal and Epidural Anesthesia. In: Sikka PK, Beaman ST, Street JA, eds. Basic Clinical Anesthesia. New York: Springer; 2015.
- ^ American Society of Anesthesiologists. Continuum of Depth of Sedation: Definition of General Anesthesia and Levels of Sedation/Analgesia. 2014; http://www.asahq.org/~/media/sites/asahq/files/public/resources/standards-guidelines/continuum-of-depth-of-sedation-definition-of-general-anesthesia-and-levels-of-sedation-analgesia.pdf. Accessed June 5, 2017.
- ^ Naidu RK, Pham TM. Pain Management. In: Sikka PK, Beaman ST, Street JA, eds. Basic Clinical Anesthesia. New York: Springer; 2015.
- ^ Memtsoudis SG, Sun X, Chiu YL, et al. Perioperative comparative effectiveness of anesthetic technique in orthopedic patients. Anesthesiology. 2013;118(5):1046-1058.
- ^ Memtsoudis SG, Danninger T, Rasul R, et al. Inpatient falls after total knee arthroplasty: the role of anesthesia type and peripheral nerve blocks. Anesthesiology. 2014;120(3):551-563.
- ^ Memtsoudis SG, Stundner O, Rasul R, et al. Sleep apnea and total joint arthroplasty under various types of anesthesia: a population-based study of perioperative outcomes. Reg Anesth Pain Med. 2013;38(4):274-281.
More on regional anesthesia