“Greening” the Operating Room and Your Budget by Reducing Desflurane Use
Cite as: Kelleher D, Fouts-Palmer EB, Yu SP, et al. “Greening” the operating room and your budget by reducing desflurane use. ASRA Pain Medicine News 2022;47. https://doi.org/10.52211/asra050122.023
This article was submitted by members of the ASRA Pain Medicine Green Anesthesia Special Interest Group.
Introduction
The harmful environmental effects of halogenated anesthetics were described as early as the 1970s, but increased global awareness of anthropogenic climate change has prompted renewed efforts to curtail their use.1-2 In the United States, inhalational anesthetics account for 1% of carbon emissions from healthcare, with desflurane having the largest impact of agents still in use.3 The Global Warming Potential (GWP) of desflurane is 15-20 times higher than that of isoflurane or sevoflurane, largely due to its longer atmospheric decomposition time.4 Furthermore, desflurane’s high minimum alveolar concentration (MAC) and low metabolism results in more agent released per MAC-hour.4 Desflurane is also the most expensive volatile anesthetic on the market.5 Not only does the inhalant cost more per bottle, but its administration also requires a heated vaporizer that must be purchased or rented from the manufacturer. Therefore, reducing desflurane use in anesthetizing locations is both financially and environmentally prudent. We describe our experience in successfully decreasing desflurane use and the environmental and financial benefits observed as a result.
Background
Our academic medical center with approximately 100 anesthetizing locations recently adopted several enhanced recovery protocols aimed at improving patient outcomes and reducing overall costs. Frequently these initiatives included novel, but expensive, medications, placing new strains on the pharmacy budget. To find ways to offset these costs, leadership from the department of anesthesiology and the perioperative pharmacy reviewed expensive and commonly used medications. During this review, desflurane was identified as a high-cost medication with no compelling evidence for use over other available agents. Additionally, sustainability-minded members of the department had been increasingly calling for the reduction of desflurane use, citing its high GWP compared to alternatives. As a result, desflurane was the first medication targeted for reduced use.
Process to Reduce Desflurane Use
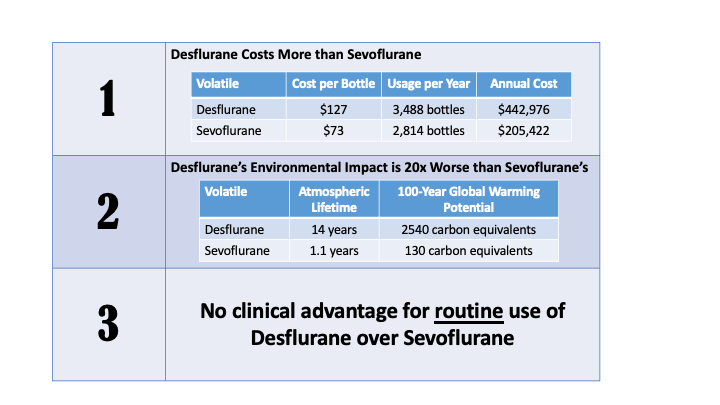
To ensure a swift and sustained reduction in desflurane use, our clinical practice committee, comprised of departmental leadership in strategy, operations, patient safety, and sustainability, developed a three-pronged strategy. First, educational information on desflurane’s environmental impact, cost, and available clinical evidence for use over other agents was presented at a department-wide conference with anesthesiologists, nurse anesthetists, and trainees in attendance (Figure 1). An email summarizing and reinforcing the main points also was sent to the department. Financial and environmental concerns were emphasized equally to appeal to both the fiscal- and environmental-minded. Second, desflurane vaporizers were removed from most anesthetizing locations, except the few commonly used for bariatric and neurologic surgery, where clinical leadership deemed desflurane use may be warranted. Several additional vaporizers remained available by request, effectively making desflurane use an “opt-in” rather than “opt-out” system. Finally, anticipating a substantial reduction in desflurane use, the supply contract was renegotiated. Originally, the contract required the purchase of at least two bottles per vaporizer per month and carried a $1,000 penalty per vaporizer return. Renegotiation allowed return of 22 vaporizers without financial penalty and reduction of the purchase minimum to one bottle per month per vaporizer. While this was expected to result in surplus desflurane, the department planned to re-allocate unneeded supplies to other hospitals in our health care system.
Figure 1. Educational information disseminated to our department.
Costs and usage are specific to our institution at the time of educational intervention. Lack of clinical indications for routine use was supported with a review of the available literature at the time of presentation. Clinicians who believed that a clinical indication existed were given the opportunity to present their counterarguments at a monthly clinical practice committee meeting.
Measuring the Impact
Procurement, purchasing, and monthly pharmacy supplies of desflurane and sevoflurane were used as metrics of anesthetic use during the one year pre- (November 2017 through October 2018) and post- (December 2018 through November 2019) intervention. Because our monthly supplies are use-based, it was considered a reasonable measure of the actual use of inhaled anesthetics. Additionally, by focusing on purchasing costs, real-time changes in the pharmacy budget for volatile anesthetics could be followed. Assuming all vapor anesthetic bottles purchased were used, total pre- and post-intervention carbon dioxide equivalent (CO2E) production was calculated using published equivalents (desflurane: 886 kg CO2E per 240 mL bottle; sevoflurane: 49 kg CO2E per 250 mL bottle).6 Data for the transitional month (November 2018) were not included.
Impact of the Initiative
Following the three-pronged intervention, desflurane purchasing decreased, with a concomitant rise in sevoflurane purchasing. Despite the rise in sevoflurane use, total purchasing costs of volatile anesthetic were reduced by $499,789 (60.9%) over one year (Figure 2), with per-case costs of volatile anesthetic reduced from $27.68 to $10.52. Estimated CO2E production also was reduced by 84.8%, from 3,970,332 to 603,468 kg CO2E (Figure 3), the equivalent of saving 378,853 gallons of gasoline.7 CO2E production per case decreased from 134 to 19.8 kg. The redistribution of excess desflurane bottles to other hospitals in our system was not tracked, and, therefore, all bottles purchased were considered used at our facility for this analysis.
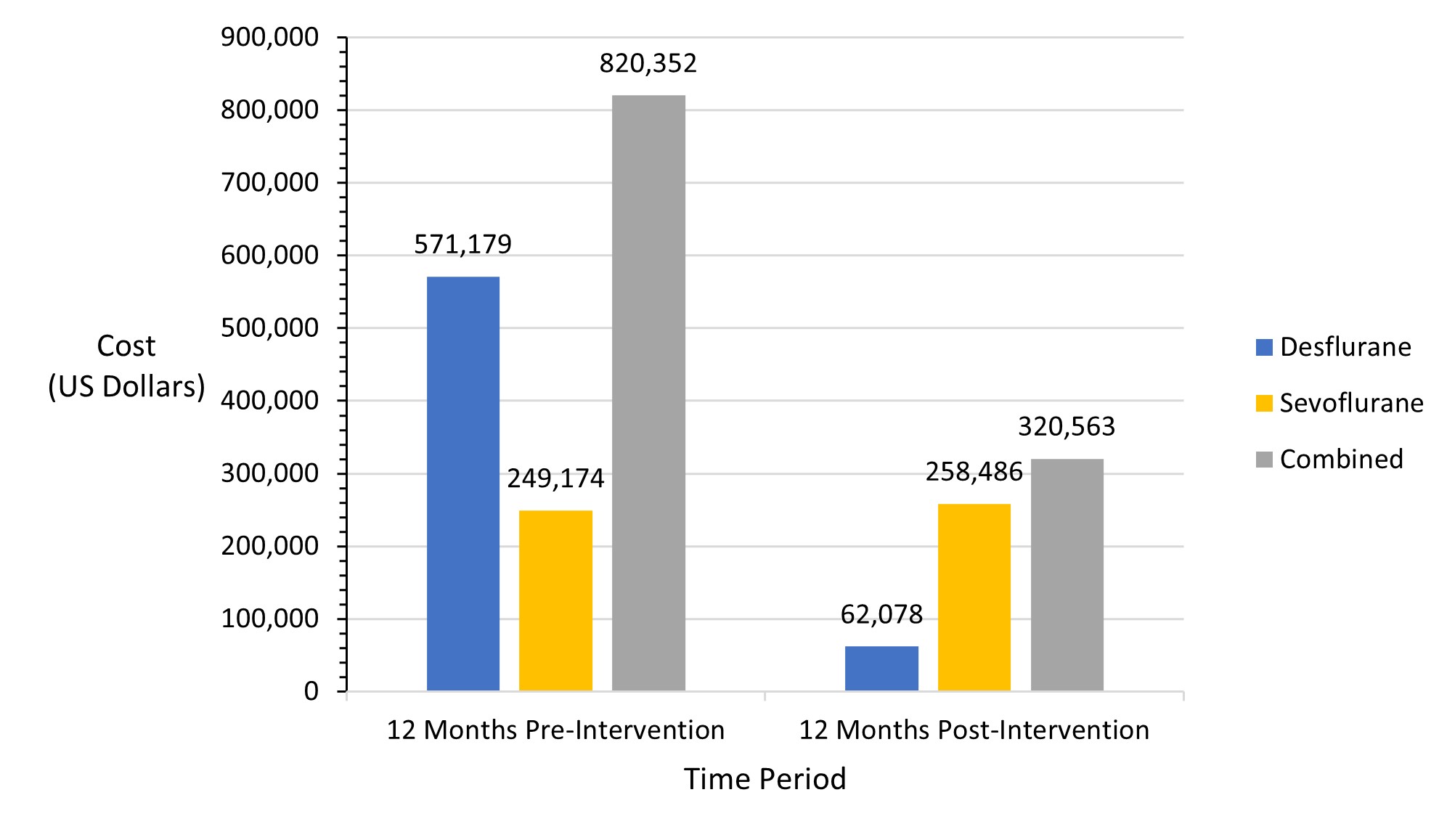
Figure 2. Total purchasing costs of desflurane and sevoflurane 12 months before and after intervention.
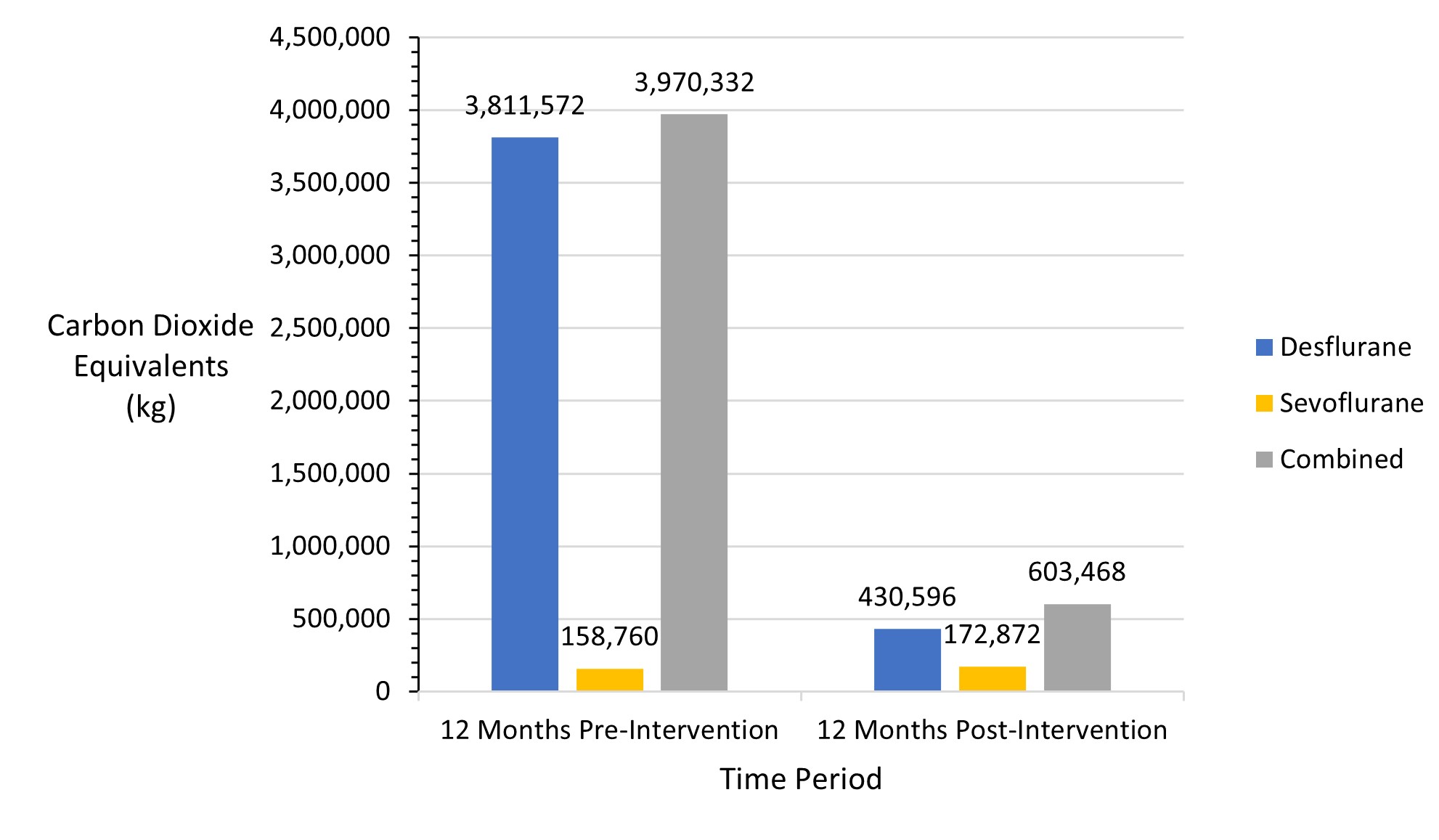
Figure 3. Total carbon dioxide equivalents (CO2E) produced before and after intervention.
Discussion
Despite past attempts by individuals to curtail the use of desflurane, our department continued to use this volatile anesthetic in large quantities, with many clinicians citing beliefs that its speed of onset and recovery minimized its financial and environmental impact compared with sevoflurane. However, by disseminating contemporary data on the financial and environmental impacts of desflurane, along with an endorsement from the departmental leadership, we were finally able to achieve the buy-in needed to effect change and achieve a substantial reduction in both pharmacy costs and carbon emissions. Faculty overwhelmingly supported the removal of desflurane vaporizers, allowing for contract renegotiation and return of vaporizers without penalty and thereby ensuring sustained effects without re-intervention. In fact, our current use of desflurane continues to decrease, as its use continues to wane. For example, many of our bariatric anesthesiologists have abandoned desflurane in favor of total IV anesthesia.
Limitations to our analysis exist. At the time of our intervention, our electronic medical record did not track actual volatile anesthetic use, and, therefore, we were forced to rely on purchasing data as a proxy. Furthermore, we only investigated changes in desflurane and sevoflurane purchasing practices, rather than considering other alternatives to desflurane, such as propofol and other IV agents. Although many people advocate for IV over inhalational anesthetics as more environmentally friendly, the focus of our educational campaign was on volatile choice during routine inhalational anesthetics.
Although restricting desflurane use to reduce cost and carbon emissions is not new, our program exhibits how a focused and systematic approach can be efficient and effective. Furthermore, identifying other methods of cost-savings, such as contract negotiation and redistribution of goods within a larger system, can lead to a greater impact than relying on individual use reduction. The cost savings realized from this intervention allowed renewed flexibility in our perioperative pharmacy budget, ensuring our department could continue to use high-value, but potentially costly, medications to optimize patient care. By collaborating with perioperative pharmacy, we were able to maintain our department’s high academic, clinical, and ethical standards, while achieving the institution’s goal of reducing overall costs.
Conflicts of Interest: The following authors declare no conflicts of interest: Deirdre C. Kelleher, E.B. Fouts-Palmer, Shao Ping Yu, and Vinod Malhotra. Patricia Fogarty Mack declares the following conflicts: Consultant for Rubin Anders, Medical malpractice defense expert for Amrity Schaub, Editorial Board Member for Journal of Perioperative Care and OR Management, Editor of a medical textbook on Problem Based Learning.

Deirdre C. Kelleher, MD, is an assistant professor of clinical anesthesiology in the department of Anesthesiology at Weill Cornell Medicine in New York, NY.
E.B. Fouts-Palmer, MD, is an assistant professor of clinical anesthesiology in the department of Anesthesiology at Weill Cornell Medicine in New York, NY.
Shao Ping Yu, MPH, is the Quality and Patient Safety manager in the department of Anesthesiology at Weill Cornell Medicine in New York, NY.
Vinod Malhotra, MD, is a professor of clinical anesthesiology in the department of Anesthesiology at Weill Cornell Medicine in New York, NY.
Patricia Fogarty Mack, MD, is an associate professor of clinical anesthesiology in the department of Anesthesiology at Weill Cornell Medicine in New York, NY.
References
- Fox JWC, Fox EJ, Villanueva R. Letter: Stratospheric ozone destruction and halogenated anaesthetics. Lancet 1975;305:864. https://doi.org/10.1016/s0140-6736(75)93048-2
- White SM, Shelton CL, Gelb AW, et al. Principles of environmentally-sustainable anaesthesia: a global consensus statement from the World Federation of Societies of Anaesthesiologists. Anaesthesia 2022;77(2)201-12. https://doi.org/10.1111/anae.15598
- Varughese S, Ahmed R. Environmental and occupational considerations of anesthesia: a narrative review and update. Anesth Analg 2021;133(4):826-35. https://doi.org/10.1213/ANE.0000000000005504
- Sherman J, Le C, Lamers V, Eckelman M. Life cycle greenhouse gas emission of anesthetic drugs. Anesth Analg 2012;114(5):1086-90. https://doi.org/10.1213/ANE.0b013e31824f6940
- Moody AE, Beutler BD, Moody CE. Predicting cost of inhalational anesthesia at low fresh gas flows: impact of a new generation carbon dioxide absorbent. Med Gas Res 2020;10(2):64-6. https://doi.org/10.4103/2045-9912.285558
- Campbell M, Pierce T. Atmospheric science, anaesthesia, and the environment. BJA Education 2015;15(4):173-9. https://doi.org/10.1093/bjaceaccp/mku033
- United States Environmental Protection Agency (EPA). Energy and the environment: greenhouse gases equivalencies calculator – calculations and references. Available at: https://www.epa.gov/energy/greenhouse-gases-equivalencies-calculator-calculations-and-references. Accessed Jan. 30, 2020.
- De Medts R, Hendrickx JF, De Wolf AM, Carette R. Sevoflurane or desflurane: which one is more expensive? Can J Anaesth 2016;63(3):358-9. https://doi.org/10.1007/s12630-015-0530-9