How I Do It: Transition Pain Clinic, Duke Health
Perioperative Challenges in Patients Taking Opioids
Patients experiencing chronic pain who are undergoing surgery present unique challenges to successful outcomes. Many in this population show tolerances to traditionally used medications, and their perioperative outcomes are heavily impacted by both dose and duration of their preoperative opioid use. We see that patients who are on high-dose opioids before surgery are at significant risk for poor outcomes, making them a high-risk group. These patients use significantly higher opioid doses for analgesia, yet continue to report worse pain control and lower satisfaction with their care.
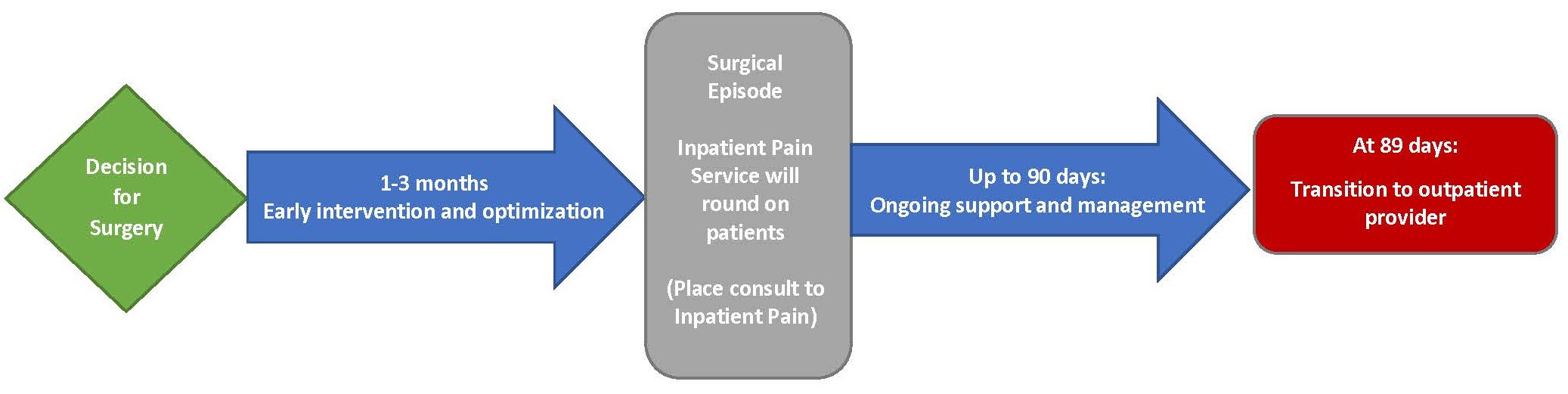
However, significant improvement in clinical outcomes can be seen in patients effectively weaned from their opioid dose prior to surgery, presenting with results similar to nonopioid users. An ideal model of care involves identification of patients on high-dose opioids, preoperative optimization of pain management regimens, and ongoing support and pain management through the patient’s hospitalization and up to 90-days following surgery. With this care model in mind, Duke Health established the Perioperative Pain Care Clinic, which is the first of its kind in the nation.The purpose of the clinic is to provide comprehensive care that starts with preoperative optimization of pain and medication management and continues this process throughout the postoperative recovery phase. The care provided in this clinic is broken down into these three phases, allowing for preoperative optimization, immediate postoperative pain control, and postoperative management and tapering.
Figure 1. Duke Health Perioperative Pain Care Clinic Phases of Care
Preoperative optimization can occur through a variety of methods. There are three key elements to an effective optimization plan: psychologic optimization, medical optimization, and physical optimization. During the postoperative period, these same methods are encouraged, allowing for optimal pain control during this time.
The Ideal Clinical Care Model
Components of preoperative optimization include opioid weaning and use of multimodal approaches to manage pain with adjuvant drugs, interventional techniques, and other modalities. The most successful approach for perioperative pain control involves a multimodal model of care that decreases opioid requirements while maintaining adequate pain control. Following preoperative optimization, a clear multimodal strategy for intraoperative and inpatient management should occur. At Duke, the pain providers who staff the Perioperative Pain Clinic also staff the Inpatient Pain Service, providing continuity of care for these patients.
Preoperative optimization can be divided into three main categories: psychological optimization, medical optimization, and physical optimization (Figure 2).
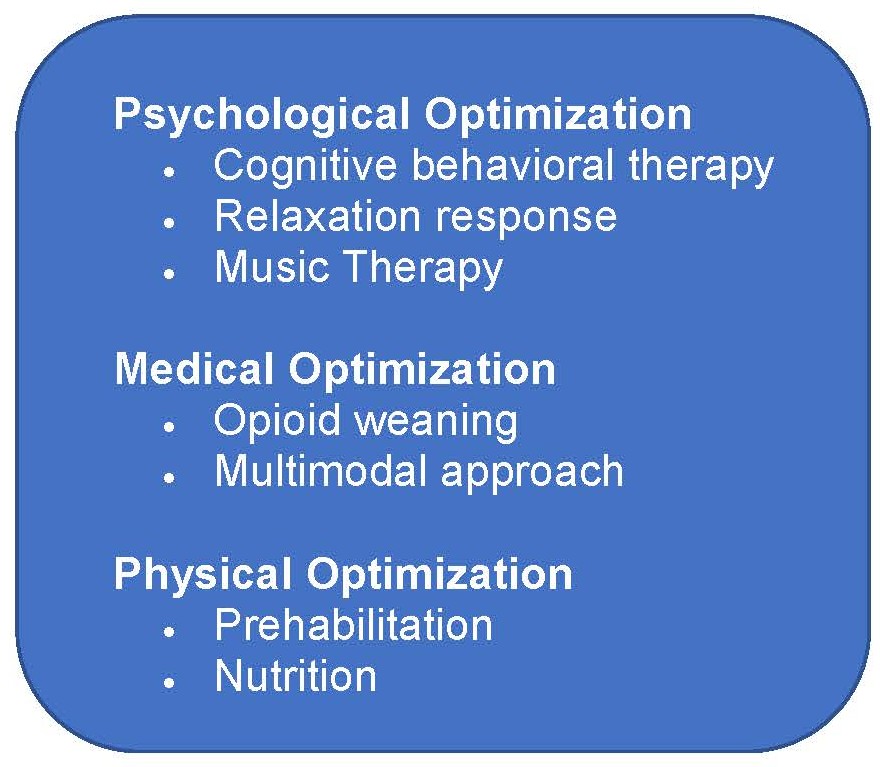
Figure 2. Key Elements of Preoperative Optimization
Psychological optimization
One of the challenges practitioners face when working to optimize a patient in pain is the patient’s perception of control over the pain. When the patient feels like they will no longer be able to control or manage their pain, whether pharmacologically or otherwise, they become hesitant in their compliance with the optimization practices. Although many techniques exist for psychological optimization, music therapy is found to have the most compliance and efficacy for patients seen in the Perioperative Pain Clinic. There is no specific type of music required for patients to listen to during music therapy, but patients should choose music that calms and relaxes them, as opposed to that which excites and stimulates them.
Medical optimization
Medical optimization is achieved by weaning opioid dosing. Opioid use during the preoperative period can be used as an independent predictor of postoperative outcomes. Opioid weaning is therefore an imperative component of medical preoperative optimization. Concurrent efforts at preoperative psychological optimization may help control the pain experienced by patients and aid in the opioid tapering process. It has been found that patients who successfully decrease preoperative opioid use have postsurgical clinical outcomes comparable to outcomes of patients with no preoperative opioid use.
Physical optimization
This optimization is achieved through proper prehabilitation and nutrition. Preoperative nutrition focuses on building a diet containing anti-inflammatory foods, decreasing physical stress on the body. This diet is mainly plant-based, consisting of produce, spices and herbs, and low-fat proteins. Patients following an anti-inflammatory diet should avoid fried or processed foods, red meats, and full-fat dairy products and they should decrease alcohol consumption. While these restrictions may seem harsh, the anti-inflammatory diet allows for a great variety of fresh fruits and vegetables, spices, nuts, fish, and chicken, among other foods.
The ideal dose reduction would entirely eliminate the need for preoperative opioid therapy; however, a 50% reduction in oral morphine equivalent (OME) administration has demonstrated improvement in post-surgical outcomes. Approaches to opioid tapering vary and are highly dependent on individual patient opioid tolerance and past experiences. A good rule of thumb is to aim for no more than a 10%-20% taper every 5-7 days, with a 25% taper considered to be an accelerated tapering regimen. Depending on the length of time between the preoperative appointment and surgery date, the standardized plan can be altered. Many patients reveal that they often routinely omit doses without adverse effects and their taper can be personalized to a more rapid decrease. As such, the weaning protocol should be individualized for each patient, an agreed upon strategy by both patient and provider.
What does this mean?
At Duke, patients who were optimized and then provided consistent follow-up post discharge care showed a trend toward better outcomes in terms of opioid dose requirement. Not only did the perioperative opioid tapering patients decrease their preoperative opioid dose, but they also displayed a significant reduction in opioid dose requirement 90-days after their procedure from their baseline dose. By equipping patients with the tools necessary to manage their pain, even acutely, they became empowered to take some control of their pain care and recovery.
Establishing and Validating the Perioperative Pain Clinic
The Perioperative Pain Clinic at Duke is staffed by an inpatient pain team of physicians and nurse practitioners. This allows for continuity of care throughout the entire perioperative period. One of the primary outcomes examined through this clinic is patient opioid use, as described. However, other outcomes reported from these clinic patients include pain scores, length of hospitalization, and emergency department visits and readmissions within 30 days of hospital discharge.
As this is a hospital-based clinic, we have great collaboration with Duke University Hospital, which provides additional support to these patients through social workers. The professional fees for this clinic do not always cover the total costs. However, it is a value-generating endeavor that may contribute to cost avoidance and improvements in fiscal margins in the long-run.

Padma Gulur, MD, is a professor of anesthesiology and population health and executive vice chair at Duke Anesthesiology and director of Pain Management Strategy and Opioid Surveillance at Duke Health in Durham, NC.
Brian Starr, MD, is an assistant professor of anesthesiology at Duke Health in Durham, NC.

Amanda Nelli, MD, is the lead postdoctorate associate of PROMIS Lab in the department of Anesthesiology at Duke Health in Durham, NC.

Leave a commentOrder by
Newest on top Oldest on top