Vertebroplasty and Kyphoplasty
Authors
Mark N. Malinowski, DO
Pain Fellow, Department of Anesthesiology
Texas Tech University Health Sciences Center
Lubbock, TX
Allen W Burton, MD
Professor and Chairman
Department of Pain Medicine
University of Texas MD Anderson Cancer Center
Houston, TX
Introduction
Vertebroplasty and kyphoplasty are spine fracture stabilization techniques that are performed for relief of pain following vertebral compression fractures (VCFs) most commonly secondary to osteoporosis. Osteoporosis is a degenerative bone disease that affects approximately 44 million people worldwide. The incidence increases with age although osteoporosis may present in any decade of life. All ethnicities are affected, however the frequency is increasing most rapidly in women of Hispanic descent.[1]
Several etiologies have been known to promote osteoclastic activity and are the basis for its classification. Primary osteoporosis can be divided into type 1, or postmenopausal osteoporosis, where estrogen deficiency may promote bone resorption, and type 2, or senile osteoporosis, which may be preceded by dietary vitamin deficiency (Vitamin D, calcium) or tissue insensitivity in the elderly. Secondary osteoporosis represents those cases where disease related hormone imbalance (hyperparathyroidism, hypogonadism) or drug-related side effects (e.g. glucocorticoids) are the cause.2
Osteoporosis is widely recognized as a cause of boney fracture. While some fractures may be minor, other fractures of the pelvis, long bones and vertebrae can have a significant impact on the physical and mental health of the patient. An overwhelming majority of these fractures result in severe pain, immobilization and debilitation.[2]
Vertebral compression fractures (VCFs) in particular are associated with significant debilitation, and the mortality rate is directly proportional to the number of VCFs.[3] By 2025, direct healthcare costs of VCFs are estimated to reach 25 billion dollars.[1] Initial treatment of VCFs includes rest, analgesics, bracing and treatment of the underlying cause (i.e., osteoporosis).
Indications
The widely accepted indications for percutaneous vertebroplasty (VP) and kyphoplasty (KP) include, but are not limited to, painful osteoporotic VCFs that continue to cause significant pain which are unresponsive to conservative management.[4-6] Pain due to neoplastic vertebral body invasion with fracture or osteonecrosis is another indication. Other more rare indications include vertebral body (VB) stabilization prior to surgical intervention, palliation of pain in inoperable vertebral tumors or secondary to fracture nonunion. VCFs rarely lead to canal compromise and myelopathy, but in such cases, prompt evaluation for surgical decompression is mandatory.[6]
Pre-Procedure Assesssment
Planning the procedure and the choice of technique not only involves a thorough history and physical examination with particular attention to the pattern of back pain, but also a careful evaluation of fracture morphology using relevant imaging (i.e., MRI) of the appropriate vertebral level (Figure 1).[7] Classification systems of VCFs are published and generally consider morphology, height, symptom chronicity and healing time.[8-9]
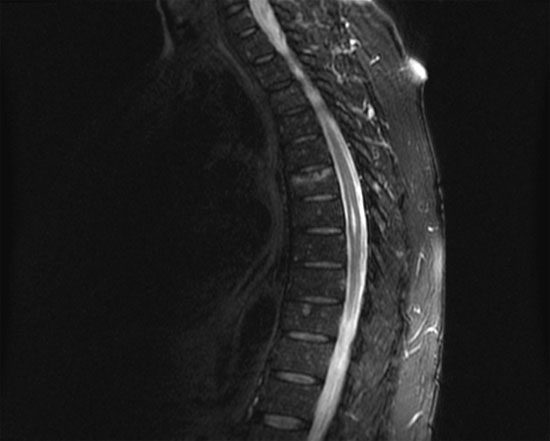
Figure 1. Image demonstrates enhancing bone edema of a typical thoracic endplate fracture on T2 weighted sagittal MRI (courtesy A Burton, MD).
Technical Consideration
Vertebroplasty is the percutanous cannulation of the vertebral body and subsequent injection of polymethylmethacrylate (PMMA). Kyphoplasty, a variation of vertebroplasty, additionally requires an inflation and deflation sequence using a “tamp” (balloon) prior to cement injection that may result in vertebral body height restoration when possible.
Vertebroplasty has progressed as a treatment for VCFs of multiple etiologies since it was first introduced by Galibert and colleagues.[4] The technique is performed under local or general anesthesia. Fluoroscopic guidance is used to guide bone biopsy needles into the vertebral body (VB) most commonly through the facet shadow identified by anteroposterior (AP) view. Specifically, the AP view is used to identify the end plate border of the VB. The pedicle shadows are aligned to the middle portion of the VB in the horizontal plane, a natural position for most vertebrae once end plates are “squared.” After proper localization of the skin and subcutaneous tissues often with lidocaine, a bone biopsy needle is driven in a coaxial fashion so as to contact the lateral aspect of the pedicle shadow (Figure 2).
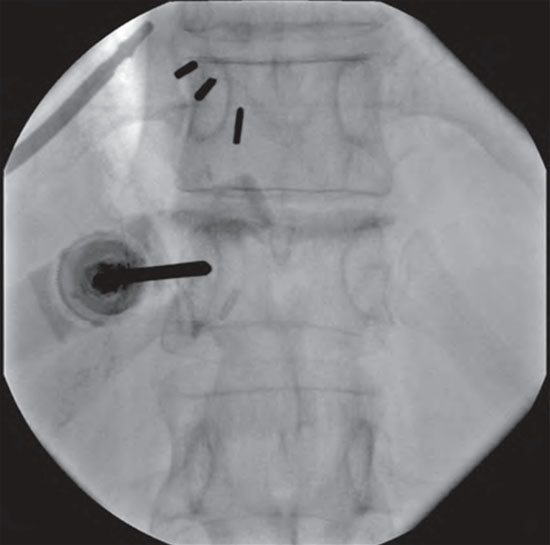
Figure 2. The transpedicular approach. The trocar is initially placed at the lateral border then advanced until it approximates the medial border (shown). The trocar tip should then be at the posterior aspect of the VB in lateral view when the medial border is approximated on AP view (Image courtesy of R Justiz, MD).
As the needle is driven deeper down the pedicle, serial AP and lateral images are used to ensure that, as the needle is advanced toward the medial pedicle border, it approximates the posterior VB border on lateral view. This technique ensures that advancement is not too medial (canal invasion), too lateral (pedicle fracture), or too inferior (nerve root injury). Once in proper position, the needle is advanced to the junction of the anterior one-third and posterior two-thirds of the VB, and radio-opaque PMMA is slowly injected under fluoroscopy to vigilantly follow cement spread, and injection is ceased when the PMMA spreads near a vital structure or into the posterior one-third of the VB.
This transpedicular approach can be performed both unilaterally and bilaterally. Similarly, where vertebral anatomical variation is of concern, an extrapedicular approach (Figure 3) can be performed such that the biopsy needle is inserted just lateral to the boney junction of the transverse process and superior articulating process. In the thoracic vertebrae, the entrance occurs medial to the corresponding costovertebral junction. A review of VP technique has been recently published.[10]
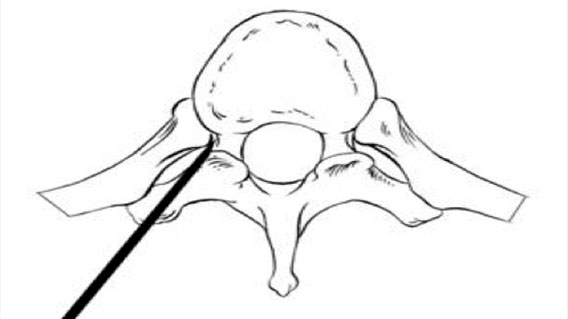
Figure 3. The extrapedicular approach in axial schematic view. The trocar is placed just lateral to the pedicle shadow but medial to the costovertebral junction.
Kyphoplasty is considered a variation of the VP technique with distinctive differences. While the approach to bone penetration is similar, the use of KP involves pressurization of the VCF with balloon “tamps” to a maximum of 220 psi. Due to the nature of the procedure, a bilateral approach is a necessity. Theoretically, creation of a cavity under pressure may allow compression of osseous fragments thereby restoring height to the VB. Some studies show that subsequent PMMA injection into that cavity is associated with less cement extravasation than VP.[28] While no direct head to head studies exist, the procedural indications overlap. Thus, a procedural comparison between VP and KP is seen in Table 1.
While the exact mechanism of analgesia is unknown, fracture stabilization is usually associated with significant pain relief, and the PMMA internal casting is felt to be the most likely mechanism of analgesia. Bone height restoration with subsequent reduction of facet related, mechanical pain and local neurolysis of nociceptors via the PMMA exothermic effect are also potential pain relieving aspects of the procedures.
| Procedure | Advantages | Disadvantages |
|---|---|---|
| Vertebroplasty |
|
|
| Kyphoplasty |
|
|
Overview of the Evidence
The efficacy of vertebroplasty has recently been the subject of much debate. A recent comprehensive review of the evidence analyzing VP and KP in the treatment of VCF related back pain was published.[7] Until its date of publication, no randomized, double-blinded, placebo controlled studies were available for analysis. Several retrospective studies have demonstrated significant improvement in overall pain scores in both osteoporotic and cancer-related VCFs following VP.[11-13] In addition, two case series suggest significant and durable improvement in VCFs secondary to multiple myeloma as well as VCFs associated with significant advanced metastatic cancer.[14-15] Several prospective studies have also demonstrated significant pain relief following VP.[7]
Both small and larger studies have evaluated the short and long term outcomes following VP.[16-18] Pain relief was consistently early after the procedure resulting in significant and lasting improvements in physical function, pain and disability from weeks to several months or years after the procedure.[16-19] In one study, McGill questionnaire findings were suggestive of worsening outcomes at a five year follow up, and this could possibly be attributed to three of twelve patients who experienced a total of four new fractures over the time period in question.[17] Additionally, a prospective, double cohort study of 101 consecutive patients who were treated by VP and 27 patients treated by conservative therapy found that preoperative pain scores and functionality improved with VP over conservative care at 3 months post-procedure.[20]
Recently, the VERTOS Study examined 34 patients who were prospectively randomized to VP or to an “optimal pain management” group. Despite prematurely aborting the study due to high cross over rates, significant pain relief and decreased analgesic use was noted by postoperative day one. However, significant difference between the groups was lost by two weeks. Although pain relief was not significantly greater over the long term, quality of life and disability was found to be significantly improved at one day and two weeks as determined by Quality of Life Questionnaire of the European Foundation for Osteoporosis (QUALEFFO) and the Roland-Morris Disability questionnaire.[21] Interestingly, Muijs and colleagues demonstrated both short- and long-term improvement in pain relief, satisfaction and functional capacity following VP as compared to controls.[22] This study was a first to provide evidence on “older” VCFs with a good longer term response rate of 80%. However, sample size and adjunct medication use in the VP group could confound its results.
Kyphoplasty has also shown significant promise, however the extent to which it has been studied is less than VP. In a recent review, two prospective case series and two retrospective reviews were examined.[7] Both prospective case series reported significant improvement in pain and physical function up to six months after KP in patients with VCFs associated with multiple myeloma or osteoporosis.[23-24] Similarly, both VP and KP demonstrated a significant reduction in pain relief post-procedure, and relief was significant from an average follow up of 4.5 months to nearly one year.[13][23]
The fracture reduction and evaluation trial (FREE), a randomized, prospective, controlled multi-center trial, evaluated 128 control and 138 KP patients with osteoporosis associated VCFs. Significant functional improvement (SF-36 PCS) in KP group was found from baseline up to 6 months, but this improvement was lost by 12 months. Similarly, days of restricted activity improved at 1 month and opioid use decreased up to 6 months, but became insignificant by 12 months in each. However, quality of life, impairment and pain (EQ-5D, RMDQ, NRS) showed significant improvement in the KP group up to 12 months. Although a numerically higher number of new fractures occurred in the KP group, the study was underpowered to detect a reportable significance. In spite of an unblended study, a non-standardized control group and a 78% follow up rate in the control group, they concluded that KP improved QOL, function, mobility and pain score more rapidly than conservative management and suggested that KP is an early option for treatment soon after fracture.[25]
Two recent publications have created some interesting controversy regarding the efficacy of VP.[27-28] Kallmes et al. published the INVEST Trial, one of the first to perform a randomized, double-blinded, placebo-controlled multi-center trial evaluating the efficacy of VP in the treatment of osteoporotic VCFs.[27] In their study, 131 patients were randomized into 2 groups, 63 of which assigned to a “simulated” procedure and 68 patients to the VP treatment group. Patients treated by “simulated procedure” were given subcutaneous injection of local anesthetic that was additionally applied to the periosteum of the corresponding pedicle. Blinded patients were subjected to physical and vocal cues such as pressure applied to their backs and exposure to the scent of mixed PMMA. Inclusion criteria were patients with up to 3 VCFs, refractory pain relief to conservative therapy, a NRS of at least 3 on a ten - point scale and a VCF age of less than 1 year as determined by pain duration or by image associated edema (MRI, bone scan) if age was indeterminate. Pre-specified primary outcomes included NRS and RMDQ scores at specific time periods up to one month. Secondary outcomes were several and included Pain Frequency Index Score, Pain Bothersome Index Score, Study of Osteoporotic Fractures-European Quality of Life 5 Dimension Scale (EQ - 5D), the use of opioids, and scores on the SF-36 PCS and MCS components. Interestingly, no significant differences were found at any time period between VP and controls. Additionally they noted that both groups had decreased pain and disability immediately after the procedure up to 1 month of which they reported an unknown etiology. However, a trend existed where a higher fraction of VP patients experienced a meaningful improvement in pain up to 1 month, but this finding was not significant.
Buchbinder and colleagues published a prospective, double-blinded, placebo-controlled evaluation of 78 patients. Controls were subjected to a “sham” procedure where subcutaneous tissue and pedicle periosteum was treated with local anesthetic.[28] Additionally, “sham” controls were exposed to the scent of mixed PMMA and subjected to the gentle tapping of the pedicle using a blunt trocar that was intended to simulate the VP procedure. Inclusion criteria were patients with back pain of less than 12 months duration in presence of up to 2 VCFs (and greater than grade 1 collapse) and MRI evidence of either edema or a fracture line. Primary outcomes were NRS at 3 months post-procedure, but follow up at 1 week, and 1 and 6 months were also studied. Assessment was made by response to mailed questionnaires. In a striking resemblance the aforementioned study, no significant differences were found between groups in overall NRS at 3 months (95% CI) or between groups in any of secondary outcomes (95% CI). These results were consistent regardless of duration of symptoms (greater than or less than 6 weeks), sex, treatment center, or presence or absence of previous vertebral fractures. They concluded that no beneficial effect of VP over sham existed in the short term (1 week) through 6 months in patients with painful osteoporotic VCFs. Although pain scores did improve independently in each group over time, no significant differences existed.
Both groups should be applauded for their efforts. Such extensive double-blinded, placebo-controlled studies are a difficult undertaking as no groups to date who have accomplished this feat. However, the complicated nature of such a study ultimately will expose potential inadvertent flaws and raise several points of contention.
First, there is no evidence to suggest that either group of investigators were treating back pain that corresponded to the level of VCF. While incident fractures can be found in patients who are asymptomatic, it is also likely that such an aged population suffers from coexisting pain generators. Therefore, without documentation of proper physical examination, correlation between VCF-associated back pain and other source are not discernible.
Next, long recruitment times in both studies and the “liberalized” criteria mentioned by Kallmes et al. are also of concern. If such excruciating VCF-related pain did exist, how can one justify including patients with NRS greater than a low score such as 3? In liberalizing the selection criteria, one cannot avoid selection bias by enrolling patients who would be willing to be treated by a “sham” procedure as opposed to intervention, especially in cases where a low pain score is reported (e.g., NRS 3/10). While it is certainly possible that the promise of crossover to the alternative group at one month could alleviate this concern, a pre-existing selection bias cannot be ruled out.[26] While the possibility of coexisting pain generators certainly exists in each group, both studies included a control group that was subjected to a procedure widely considered to be a treatment among interventional pain physicians. While the groups intended to provide a control or sham procedure, they actually performed a medial branch that could explain the pain relief seen in the sham group(s).
While most supporting evidence comes from case reports, prospective and retrospective reviews and cohort studies, the publication of the two aforementioned ‘negative’ studies should not categorically divest the role of VP and KP to treat VCF-associated back pain. On the contrary, these studies raise important questions into the limitations of evidence-based medicine. Should patients be denied a pain relieving procedure simply because flawless studies cannot be designed? In truth, further investigation into their efficacy is warranted. However, major decisions that ultimately influence the availability of these procedures must be temporarily postponed until the evidence outweighs common sense.
Summary
Vertebroplasty and kyphoplasty are relatively new minimally invasive procedures used to treat painful vertebral fractures. Complication rates are low and overall outcomes are good. Recent controversy has occurred with two widely publicized “negative” vertebroplasty trials (i.e. procedure not better than placebo), however the authors view these trials as thought provoking, but flawed as outlined in the discussion above. Both vertebroplasty and kyphoplasty offer meaningful pain relief to patients with painful vertebral compression fractures of varying etiologies.
References
- National Osteoporosis Foundation. www.nof.org
- Heaney R. Pathophysiology of osteoporosis. Endocrin Metabol Clin North Am. 1998; 27: 255-265.
- Kado D, Browner W, Palermo L, Nevitt M, Genant H, Cummings S. Study of Osteoporotic Fractures Research Group Arch Intern Med. 1999; 159:1215-1220.
- Galibert P, Deramond H, Rosat P, Le Gars D. [Preliminary note on the treatment of vertebral angioma by percutaneous acrylic vertebroplasty.] [Article in French] Neurochirurgie 1987; 33:166-8.
- Lieberman IH, Dedeney S, Reinhardt M, Bell G. Initial outcome and efficacy of kyphoplasty in the treatment of painful osteoporotic vertebral compression fractures. Spine 2001; 26: 1631–1638.
- McGraw J, Cardella J, Barr J, Mathis J, Sanchez O, Schwartzberg M, Swan T, Sacks D. Society of interventional radiology quality improvement guidelines for percutaneous vertebroplasty. J Vasc Interv Radiol 2003; 14: 827- 831.
- Burton AW, Rhines L, Mendel E. Vertebroplasty and kyphoplasty: a comprehensive review. Neurosurg Focus 2005; 18:1- 9.
- Genant H, Wu C, van Kuijk C, Nevitt M. Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res. 1993; 8: 1137–1148.
- Lyritis GP, Mayais B, Tsakalakos N, Lambropoulos A, Gazi S, Karachalios T, Tsekoura M, Yiatzides A. The natural history of the osteoporotic vertebral fracture. Clin Rheumatol. 1989; 8: 66–69.
- Syed M, Shaikh A. Vertebroplasty: A systemic approach. Pain Physician 2007; 10:367–380.
- Grados F, Depriester C, Cayrolle G, Hardy N, Deramond H, Fardellone P. Long term observations of vertebral osteoporotic fractures treated by percutaneous vertebroplasty. Rheumatology 2000; 39: 1410–1414.
- Barr J, Barr M, Lemley T, McCann R. Percutaneous vertebroplasty for pain relief and spinal stabilization. Spine 2000; 25: 923–928.
- Fourney D, Schomer D, Nader R, Chlan-Fourney J, Suki D, Ahrar K, Rhines L, Gokaslan Z. Percutaneous vertebroplasty and kyphoplasty for painful vertebral body fractures in cancer patients. J Neurosurg Spine 2003; 98: 21-30.
- Chakrabarthi I, Burton AW, Rao G, Feiz-Erfran I, Hlatky R, Rhines L, Mendel E. Percutaneous vertebroplasty of myelomatous compression fracture in the presence of previous posterior instrumentation. J. Neurosurg Spine 2006; 5: 1–4.
- Burton AW, Reddy S, Shah H, Tremont-Lukats I, Mendel E. Percutaneous vertebroplasty–A technique to treat refractory spinal pain in the setting of advanced metastatic cancer: A case series. J. Pain Symp Mgmt 2005; 30: 87–95.
- Cortet B, Cotton A, Boutry N, Flipo R, Duquesnoy B, Chastenet P, Delcambre B. Percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fractures: an open prospective study. J Rheumatol 1999; 26: 2222–2228.
- Perez–Higueras A, Alvarez L, Rossi R, Quinones D, Al-Assir I. Percutaneous vertebroplasty: long- term clinical and radiological outcome. Neuroradiology 2002; 44: 950–954.
- McGraw J, Lippert J, Minkus K, Rami P, Davis T, Budzik R. Prospective evaluation of pain relief in 100 patients undergoing percutaneous vertebroplasty: results and follow up. J Vasc Interv Radiol 2002; 13: 883–886.
- Zoarski G, Snow P, Olan W, Stallmeyer M, Dick B, Hebel R, De Deyne M. Percutaneous vertebroplasty for osteoporotic compression fractures: quantitative perspective evaluation of long term outcomes. J Vasc Interv Radiol 2002; 13: 139-148.
- Alvarez L, Alcaraz M, Perez-Higueras A, Granizo J, de Miguel I, Rossi R, Quinones D. Percutanous vertebroplasty: Functional improvements in patients with osteoporotic compression fractures. Spine 2006; 31: 1113–1118.
- Voormolen M, Mali W, Lohle P, Fransen H, Lampmann L, van der Graaf Y, Juttmann J, Janssens X, Verhaar H. Percutaneous vertebroplasty compared with optimal pain medication treatment: Short term clinical outcome of patients with subacute or chronic painful osteoporotic vertebral compression fractures. The VERTOS study. Am J Neuroradiol 2007; 28: 555-560.
- Muijs S, Nieuwenhuijse M, Van Erkel A, Dijkstra P. Percutaneous vertebroplasty for the treatment of osteoporotic vertebral compression fractures: Evaluation after 36 months. J Bone Joint Surg. (Br) 2009; 91B: 379–384.
- Ledlie J, Renfro M. Balloon kyphoplasty: one year outcomes in vertebral body height restoration, chronic pain and activity levels. J Neurosurg Spine 2003; 98: 36-42.
- Lieberman I, Dedeney S, Reinhardt M, Bell G. Initial outcome and efficacy of kyphoplasty in the treatment of painful osteoporotic vertebral compression fractures. Spine 2001; 26: 1631–1638.
- Wardlaw D, Cummings S, Meirhaeghe J, Bastian L, Tillman J, Ranstam J, Eastell R, Shabe P, Talmadge K, Boonen S. Efficacy and safety of balloon kyphoplasty compared with nonsurgical care for vertebral compression fractures (FREE): a randomized controlled trial. Lancet 2009; 373: 1016–1024.
- Kallmes D, Comstock B, Heagerty P, Turner J, Wilson D, Diamond T, Edwards R, Gray L, Stout L, Owen S, Hollingoworth W, Ghdoke B, Annesley- Williams D, Ralston S, Jarvik J. A randomized trial of vertebroplasty for osteoporotic spinal fractures. N Engl J Med. 2009; 361: 569- 579
- Buchbinder R, Osborne R, Ebeling P, Wark J, Mitchell P, Wriedt C, Graves S, Staples M, Murphy B. A randomized trial of vertebroplasty for painful osteoporotic vertebral fractures. N Engl J Med. 2009; 361: 557-568.
- Philips F, Wetzel T, Lieberman I, Campbell-Hupp M. An in vivo comparison of the potential for extravertebral cement leak after vertebroplasty and kyphoplasty. Spine 2002; 27: 2173–2178.
Leave a commentOrder by
Newest on top Oldest on top