How I Do It: Identifying Saphenous Nerve Sonoanatomy
This article originally appeared in ASRA News, Volume 12, Number 1, pp 10-12 (February 2012).
Authors
Henning L. Andersen, MD
Consultant Anesthesiologist
Coordinating Research Department
Frederiksberg Hospital
Copenhagen University Hospital, Denmark
Andrew T. Gray, MD, PhD
Professor of Clinical Anesthesia
University of California, San Francisco
San Francisco General Hospital
San Francisco, CA
Section Editor: Steve Orebaugh, MD
Introduction
The saphenous nerve is the largest and longest branch of the femoral nerve. It is considered part of the posterior division of the femoral nerve. The adductor canal (canalis adductorius; Hunter’s canal) is an aponeurotic tunnel in the middle third of the thigh, extending from the apex of the femoral triangle to the opening in the adductor magnus.[1] The vastoadductor membrane is a continuum of the aponeurotic roof of the adductor canal that covers the distal part of the canal. The thickness of this membrane varies greatly.[2] The saphenous nerve usually exits the adductor canal at the distal end of the vastoadductor membrane or can pierce it.
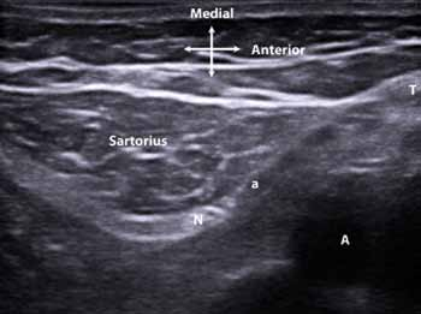
Figure 1. Distal and medial to the adductor canal near the superior-most aspect of the patella. Saphenous nerve (N). Popliteal artery (A) and vein. Saphenous branch of the descending genicular artery (a). Tendon of the adductor magnus muscle (T).
After the saphenous nerve exits the adductor canal, it travels with the saphenous branch of the descending genicular artery just beneath the sartorius muscle from the anterior to the posterior edge of the muscle (Fig 1).[3-5] This occurs where the femoral artery descends through the adductor hiatus into the popliteal fossa. At this point the saphenous nerve crosses over the tendon of the adductor magnus muscle that is interposed between the nerve and femoral artery as the nerve exits the canal (Fig 2).[3]
The saphenous nerve can divide either in the adductor canal or distal to the adductor canal in the subsartorial fat.[6] It gives off the infrapatellar branch and other cutaneous nerve branches that, in some individuals, anastomose with cutaneous branches from the obturator nerve and the medial cutaneous nerve of the thigh to form a subsartorial plexus.[6-8] The infrapatellar branch can either run parallel to the saphenous nerve or pierce the distal part of the sartorius muscle. The saphenous nerve consistently emerges into the subcutaneous tissue between the tendons of the sartorius and gracilis muscles.[9,10] The saphenous nerve will then join the undersurface of the saphenous vein in the proximal leg and follow its distal course. Medial crural cutaneous branches of the saphenous nerve will provide sensory innervation to the medial leg.
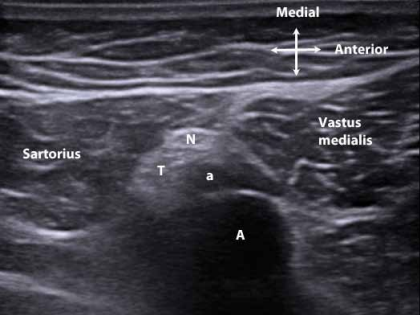
Figure 2. At the distal end of the adductor canal where the saphenous nerve (N) exits the canal crossing over the tendon of the adductor magnus muscle (T). Femoral artery (A) and vein. Descending genicular artery (a).
The posterior articular branch of the obturator nerve either enters the distal part of the adductor canal or penetrates the adductor magnus muscle on its way to the posterior knee capsule in the popliteal fossa.[6-8,11] This nerve branch could potentially contribute to the analgesic effect of the adductor canal blockade after knee surgery. However, the description of the course of the nerve in the distal part of the thigh and its relation to the adductor canal varies greatly, and the nerve may not have any significant clinical role following saphenous nerve blocks in the thigh.
The medial branch of the nerve to vastus medialis travels with the saphenous nerve at the mid-thigh level under the sartorius muscle, anterolateral to the femoral artery, in the vastus medialis muscle or just under the muscle fascia.[12,13] This nerve branch terminates in the knee capsule.[6,7,13]
Only a few of the nerves of the subsartorial plexus, namely the saphenous nerve and branches from the nerve to the vastus medialis muscle, can usually be identified with certainty by ultrasound imaging. Additionally, it is still uncertain to what extent all the plexus or just the saphenous nerve and its branches are involved in the saphenous nerve block in the adductor canal (Fig 3).
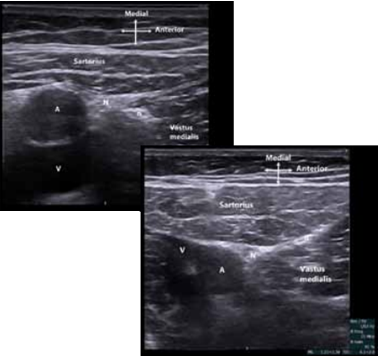
Figure 3. At mid-thigh level: Saphenous nerve and branches (N) in the adductor canal. Femoral artery (A) and vein (V). A nerve branch of the nerves to the vastus medialis muscle (n) lying in the muscle (top image) and just under the muscle fascia (bottom image).
Suggested Technique (1)
Ultrasound imaging can be used to guide saphenous nerve block anywhere along its course, so the choice of approach is somewhat arbitrary. However, we typically do not choose the distal part of the adductor canal in order to minimize the risk of nerve puncture, paresthesia, or even nerve entrapment. This level is where the saphenous nerve is least mobile and to a variable degree fixed in the vastoadductor membrane.[14] Furthermore, we have found the suggested techniques described here to be highly efficacious, safe, and robust within the broad spectrum of clinical practice.
Place the ultrasound machine on the opposite side of the bed so that the block site and display are both in front of the operator. Perform the saphenous nerve block with the sartorius muscle viewed in short axis while advancing the needle in the plane of imaging. The preferred direction is from the anterior side at the level of the mid-thigh just proximal to the take-off of the nerve and artery to the vastus medialis muscle. Because of the relatively-steep angle of insertion through the sartorius muscle an echogenic needle is typically selected with this approach.
The needle is placed through the sartorius muscle to enter the plane deep to the muscle (a trans-sartorial approach). There can be a loss-of-resistance as the needle tip crosses the vastoadductor membrane. Three to 5 mL of local anesthetic is injected within this plane, adjacent to the femoral artery. Initially the bevel of the needle faces the transducer to improve needle tip visibility. To extend the distribution under the sartorius muscle the needle can be rotated 180 degrees (bevel down) and then slowly advancing the needle towards the artery while lifting (retracting) the subsartorial fascia as gentle pressure is maintained on the injection syringe. The goal is to separate (or nearly separate) the femoral artery from the sartorius muscle.
The leg can be flexed at the knee and externally rotated to facilitate the sartorial coverage of the saphenous nerve and femoral artery, but this is not absolutely necessary and can be difficult in some patients, especially under postoperative circumstances. A similar effect can be achieved by performing the block more proximally.
Suggested Technique (2)
Another approach can be used that both provides excellent needle tip visibility and minimizes the risk of vascular puncture. An in-plane, short axis view approach almost parallel to the transducer can be used through the superficial part of the vastus medialis muscle in a lateral to medial direction overshooting the femoral artery deep to the sartorius muscle and the vastoadductor membrane (Fig 4). The advantage is that this needle track avoids directing the needle towards the femoral artery , and it improves needle tip visibility by pointing the needle tip posteriorly. Also, advancing through the fascia, coupled with loss of resistance as the needle bypasses the artery into the most superficial part of the adductor canal, may reduce the risk of puncturing the artery. The needle tip can then be placed next to the saphenous nerve. The optimal volume of injectate is currently unknown, but we recommend 15 mL within the canal.
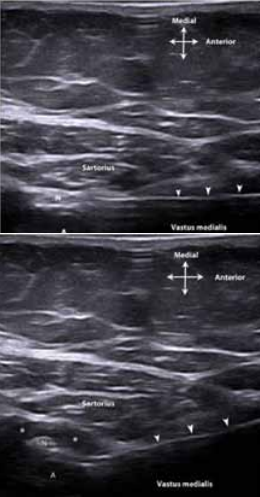
Figure 4. Needle approach at mid-thigh level: In this individual, the saphenous nerve (N) is positioned medial to the femoral artery (A) high in the adductor canal. Top image: The needle approach (arrowheads) is almost parallel to the transducer aiming over the artery. Bottom image: After penetration of the vastus medialis muscle fascia the needle (arrows) is placed at the desired position next to the saphenous nerve (N) and femoral artery (A) and the injectate (**) spreads in a semi-lunar fashion around the nerve and artery while displacing the femoral artery deeper in the adductor canal.
Assessment
There are several sonographic signs of successful saphenous nerve block in the adductor canal. The distribution around the saphenous nerve can be assessed in short and long axis views. The injectate should spread in a semilunar fashion on the anteromedial aspect of the femoral artery and saphenous nerve, with displacement of the femoral artery. If the sartorius muscle is lifted extensively, before the femoral artery is displaced, then the needle tip is probably not in the adductor canal and the needle should be repositioned. The nerve should appear brighter after the injection because of the acoustic enhancement from the surrounding injectate. The saphenous nerve can be seen to move from the side of the femoral artery to its top surface as the probe slides from proximal to distal. This is most clearly seen after injection of local anesthetic for regional block.
After most approaches to saphenous nerve block the medial leg and foot will show signs of cutaneous anesthesia. The distal boundary of sensory blockade often extends to the base of the great toe.[15]
Catheter Placement
An indwelling catheter can be placed in the adductor canal after a bolus injection at the mid-thigh level. However, the abundant amount of connective tissue in the canal makes advancement of the catheter beyond a few centimeters difficult. The placement of the catheter can sometimes be visualized by ultrasound, after the needle has been removed, to adjust the position of the catheter tip next to the saphenous nerve or femoral artery. Ensuring a free flow through the catheter while expanding the canal confirms catheter placement in the canal.
Complications
Because of the proximity of the saphenous nerve to the femoral artery, there is an inherent risk of vascular puncture when advancing the needle tip toward to the nerve. Patients with failed or partially effective saphenous nerve blocks will often report postoperative pain localized to the medial ankle, even if the surgical procedure on the lower extremity did not involve a surgical incision on the medial leg. For this reason, many believe that the innervation of the saphenous nerve includes not only cutaneous branches but also articular branches to the ankle joint and related structures deep to the skin. The clinical observation is that the addition of a saphenous nerve block to the sciatic nerve block as a rescue after ankle surgery has a surprising effect that is difficult to justify by the cutaneous distribution alone. It is theoretically possible to place the needle tip through or into one or more nerve branches during saphenous nerve block in the mid-thigh.
Although nerves to the vastus medialis muscle lie within the subsartorial plane, studies have found no measurable motor block from saphenous nerve blocks performed in this location.[16-18] A recent case series investigating the continuous saphenous nerve block after total knee arthroplasty (TKA) showed no clinically-apparent motor blockade while weight-bearing.[17]
Additional Comments
Ultrasound identification of nerves and other anatomic structures are best illustrated under real time dynamic scanning. Videos of the saphenous nerve in the adductor canal and related structures can therefore be studied with great advantage.
References
- Gray H, Lewis W H. Anatomy of the human body. Bartleby.com, S.l. 2000.
- Tubbs RS, Loukas M, Shoja MM, Apaydin N, Oakes WJ, Salter EG. Anatomy and potential clinical significance of the vastoadductor membrane. Surg Radiol Anat. 2007 Oct;29(7):569-73. Epub 2007 Jul 7. PMID: 17618402
- Scheibel M T, Schmidt W, Thomas M, Von Salis-Soglio G. A detailed anatomical description of the subvastus region and its clinical relevance for the subvastus approach in total knee arthroplasty. Surg Radiol Anat 2002; 24(1): 6-12.
- Krombach J, Gray AT. Sonography for saphenous nerve block near the adductor canal. Reg Anesth Pain Med 2007;32:369-70. PMID: 17720129
- Tsui BC, Ozelsel T. Ultrasound-guided transsartorial perifemoral artery approach for saphenous nerve block. Reg Anesth Pain Med. 2009 Mar-Apr;34(2):177-8. PMID: 19282716
- Horner G, Dellon AL. Innervation of the human knee joint and implications for surgery. Clin Orthop Relat Res. 1994 Apr;(301):221-6. PMID: 8156678
- Gardner E. The innervation of the knee joint. Anat Rec 1948; 101(1): 109-130.
- Standring S, Gray H. Gray's Anatomy, The Anatomical Basis of Clinical Practice. Churchill Livingstone, London 2008.
- Hunter LY, Louis DS, Ricciardi JR, O'Connor GA. The saphenous nerve: its course and importance in medial arthrotomy. Am J Sports Med 1979 Jul-Aug;7(4):227-30. PMID: 474860
- Arthornthurasook A, Gaew-Im K. Study of the infrapatellar nerve. Am J Sports Med 1988; 16(1): 57-59.
- Kumka M. Critical sites of entrapment of the posterior division of the obturator nerve: anatomical considerations. J Can Chiropr Assoc 2010; 54(1): 33-42.
- Thiranagama R. Nerve supply of the human vastus medialis muscle. J Anat 1990;170:193-198.
- Jojima H, Whiteside L A, Ogata K. Anatomic consideration of nerve supply to the vastus medialis in knee surgery. Clin Orthop Relat Res 2004;(423): 157-160.
- Kalenak A. Saphenous nerve entrapment. Operative Techniques in Sports Medicine 1996; 4(1): 40-45.
- Benzon HT, Sharma S, Calimaran A. Comparison of the different approaches to saphenous nerve block. Anesthesiology 2005;102:633-8. PMID: 15731603
- Davis J J, Bond T S, Swenson J D. Adductor canal block: more than just the saphenous nerve? Reg Anesth Pain Med 2009; 34(6): 618-619.
- Lund J, Jenstrup M T, Jaeger P, Sorensen A M, Dahl J B. Continuous adductor-canal-blockade for adjuvant post-operative analgesia after major knee surgery: preliminary results. Acta Anaesthesiol Scand 2011; 55(1): 14-19.
- Saranteas T, Anagnostis G, Paraskeuopoulos T, Koulalis D, Kokkalis Z, Nakou M, Anagnostopoulou S, Kostopanagiotou G. Anatomy and clinical implications of the ultrasound-guided subsartorial saphenous nerve block. Reg Anesth Pain Med. 2011 Jul-Aug;36(4):399-402. PMID: 21697687
Leave a commentOrder by
Newest on top Oldest on top